INTRODUCTIONIn the early of XX century, tumor surgical approach on sellar areas was considered a challenge for neurosurgeons due to a high risk of lesions on adjacent neural and vascular structures, though not recommended.
Therefore, once Guiot(1,3) and Hardy(2) have modernized and standardized the surgery approach, it has been considered the safest and most effective way of treatment. Since then, transphenoidal surgery has been highly used by neurosurgeons worldwide.
Guiot(1) was also the first one to use endoscopes, intending to change transphenoidal surgery even less invasive. In the past, the use of endoscopes was to identify normal pituitary gland and residual tumor(4,5). Advanced techniques by ENT doctors on paranasal sinus surgery by endoscopic approach(6-9), endoscopic transphenoidal surgery has gained power. Besides, there was a trend towards using endonasal way(10-14) in detriment of trans-septal ways(15,16) due to the low number of complications related to the procedure(12).
Thus, it has been 10 years since Jho(5) and others have been making great efforts to improve such technique. By by studying corpse dissection and creating specific surgery tool, the transphenoidal surgery through endoscopic approach has been considered the first choice for sellar tumor treatment(10-16), and also it has been showing low rates of mortality or morbidity(10-18).
Although there are so many advances, the procedure is not risk-free(19-21). Hemorrhages is a scary complication, and although they rarely occur, they can be severe and deadly(18-22). They are divided into two great groups according to anatomical structure(18):
1. Sphenoid and nasal complications;
2. sella turcica complications.
Kassan and cols(22) also suggested other simple and objective ways for the same purpose:
1. Venous and artery bleeding;
2. Low or high flow bleeding.
There are other three extremely important details to be considered:
1. which of the affected tissue: bone, meninges, tummor, brain tissue;
2. what neurovascular structures are related to hemorrhage focus;
3. which of the affected dissection area: intradural or extradural.
Hemorrhage of any type must be considered in particular way and, different factors should also be analyzed before choosing the proper haemostatic technique. In the current study, it is described the administration of those complications and also results with the use of different tools devoted to such surgery, such as appropriate instruments and haemostatic sponges and gelatin foams (SPONGOSTAN powder
®).
MATERIAL AND METHODS From March 2001 to December 2005, 95 patients were submitted to endoscopic endonasal approach in order to have their hypophysis tumor ressected. In a 20-patient group, specific haemostatic products were used for low flow bleeding (Spongostan
®, fibrillar Surgicel
®) and bipolar forceps devoted to endonasal surgery (TAKE-APART
® Bipolar Forceps - Karl Storz, Gmbh). In these 20 cases, other haemostatic techniques such as saline solution irrigation at 40ºC, bone wax or drilling were not used, with the purpose to evaluate the effectiveness of haemostatic tools. Intra-operative bleeding control as well as occurrences and quantity on post-surgery period were also observed.
Patients underwent operation under total endovenous general anaesthesia with Propofol
® and Fentanil
®. After anaesthesia, they were placed in dorsal recumbent in mild proclivity and with semi-bended head which made a light rotation movement possible. During surgery the average blood pressure remained between 55 and 70 mmHg.
Bipolar bleeding quantification during intra-operative period was determined by the surgeon. Light bleeding was considered when hemorrhage amount neither affected endoscopic vision nor lengthened surgery time; moderate bleeding was considered when hemorrhage amount affected endoscopic vision but did not lengthen surgery time; severe bleeding when hemorrhage affected endoscopic vision and implicated procedure by lengthening surgery time (over 90 min). In order to control bleeding, it was used cautery knife (for high flow, intra or extradural bleeding) and haemostatic sponges - Spongostan
® (for low flow bleeding on extradural place). Fibrin glue has not been used, and surgery average time was 74 min.(52-133).
After surgery, patients remained resting for 24 hours with a light bandage over their nostrils. Bleeding was considered light when there was no need of bandage changes; moderate when bandage changes were needed and severe one when there was need of nasal packing by using Foley probe.
RESULTSData regarding age, gender, type of hypophysial tumor and bleeding are displayed in Table 1.
In any of the cases there was need of surgery interruption due to bleeding. In eight cases, light nose bleeding was reported with spontaneous remission for 72 hours. Late moderate bleeding occurred in one case, and it was associated to the use of antiagregant medication.
DISCUSSION Since 1922, when Walter Dandy(24) first brought up neuroendoscopy approach, several technological advances and improvement of the surgery technique have been helping neurosurgeons on treating sellar tumors by endoscopic approach, and, nowadays, neuroendoscopic approach has been largely applied worldwide.
There are basically two ways of neuroendoscopic access(22): expanded endonasal access and the transcortical accesses. Just as in a microsurgery, the haemostasis is fundamental for a satisfactory surgical result. It is important to highlight that the technical principle of neuroendoscopic haemostasis is identical to the microsurgery(22).
Bleeding during surgery process by endonasal endoscopy is related to clinical, technical and anatomical factors. As one might know, hypophysial tumors, especially the secretory adenomas, are associated to several systemic clinical alterations such as artery hypertension and diabetes mellitus, in such a way that its intra-operative handling can be difficult and hemorrhage complications are hard to be controlled.
Technically speaking, surgery administration of mucosas, friable and irrigated tissues is always associated to severe bleeding, as reported in the current series. In acromegalic patients, hypertrophy of the nasal turbinate presented technical difficulties by reducing work space. In the same way, bone and cartilaginous tissues in the septum of the nose and anterior wall of sphenoid are bleeding place. The opening of sella turcica exposing dura-mater and peridural space is also associated to bleeding (Picture 1). As the source of such bleedings is diffuse and of low flow, the use of jelly-consistence-like haemostatic products (Spongostan
®) provides advantages by penetrating and working on irregular sinusal salience (Pictures 2 and 3).
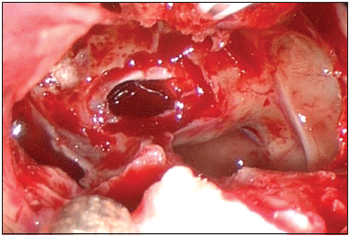
Picture 1. Peridural bleeding in the interior of sphenoid sinus.
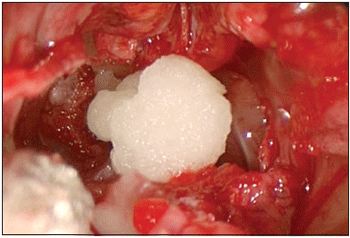
Picture 2. Application of haemostatic gelatine (Spongostan powder
®).
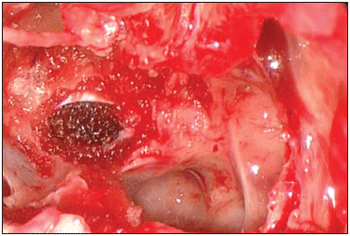
Picture 3. Final aspect.
The Spongostan
® is a haemostatic solution made from collagen mixed to jelly foam which comes from pigs. After being soaked in saline solution with the help of a serynge, the sponge is placed on extradural and low-flow bleeding places. Such sponge is able to control bleeding by activating coagulation cascade, but especially, by absorbing the amount of blood over 40 times its own weigh. Besides, haemostasis is made without the occlusion of the affected vessel. The use of the sponge was effective on controlling patients' bleedings. It is bioabsorbable and able to be active for around four or six weeks.
High flow artery bleeding occurs due to accidental lesion of the septal artery (on the ostium of the sphenoid sinus)(11) and of the internal carotid artery (on lateral sellar opening and during tumor removal)(26). In the first case, the use of bipolar or monopolar coagulation is sufficient. Therefore, carotid lesion is considered the worst of the complications. According to other studies(18,22,25), bipolar cautery knife(22) or packing of lesion and subsequent endovascular treatment(18,25) can be used in this situation.
The bipolar cautery knife(22), is the most important haemostatic instrument used on neuroendoscopy. It is used to soothe minimize thermal lesion in nearby structures, and also in any kind of bleeding, unlikely the cautery knife, which can never be used either on the base (sphenoid sinus) or on the interior of the cranium due to heat dissipation and then to thermal lesion. Among all haemostatic techniques, there is still the irrigation with saline solution in adequate temperature (40º C)(26) and bone wax. Irrigation with saline solution is extremely effective and should be used as adjuvant in any kind of bleeding. Bone bleeding can be easily controlled with saline irrigation, bone wax or drilling of the affected area. Bleeding from dural sinus was better controlled with local applications of microfibrilar collagen(23).
CONCLUSIONHaemostatic control is the key for any surgical procedure. Regarding endoscopic endonasal surgery, due to its own features, a proper approach and bleeding control is imperative for a successful result. That's why a special care should be taken into consideration towards any type of bleeding during surgery.
Recognizing the type of bleeding (low or high flow bleeding) and hemorrhage place and source (intradural, extradural) is fundamental for the right treatment, and the surgery team must be ready for those situations. The use of mono or bipolar cautery knife is completely necessary on high flow bleeding. Yet, for low flow bleeding, the use of haemostatic sponges is recommended, especially on extradural spaces and on paranasal and nasal cavities.
Though, endonasal endoscopy approach should be performed by using proper tools. Haemostasis must be under especial attention by surgeon, by considering this approach an invasive one.
REFERENCES1. Guiot G, Rougerie J, Fourestier M, Fournier A, Comoy C, et al. Une nouvelle technique endoscopique: Exploration endoscopiques intracraniennes. Press Medical 1963; 71:1225-1228.
2. Hardy J. Transsphenoidal microsurgery of the normal and pathological pituitary. Clinical Neurosurgery 1969; 16:185-214.
3. Guiot G, Derome P. Surgical problems of pituitary adenomas. In: Krayembuhl (ed). Advances and technical standards in Neurosurgery. Vienna: Springer, 1976:3-33.
4. Gamea A, Fathi M, El Guindy A. The use of the rigid endoscope in trans-sphenoidal pituitary surgery. Journal of Laryngology and Otology 1994; 108:19-22.
5. Jho HD, Carrau RL. Endoscopy assisted transsphenoidal surgery for pituitary adenoma. Technical note. Acta Neurochirurgica (Wien) 1996; 138:1416-1425.
6. Senior BA, Kennedy DW, Tanabodee J, Kroger H, Hassab M, et al. Long-term results of functional endoscopic sinus surgery. Laryngoscope 1998; 108:151-157.
7. Kennedy DW. Functional endoscopic sinus surgery. Technique. Archives of Otolaryngology 1985; 111:643-649.
8. Kennedy DW, Zinreich SJ, Rosenbaum AE, Johns ME. Functional endoscopic sinus surgery. Theory and diagnostic evaluation. Archives of Otolaryngology 1985; 111:576-582.
9. Messerklinger W. Background and evolution of endoscopic sinus surgery. Ear Nose Throat Journal 1994; 73:449-450.
10. Jho HD, Carrau RL. Endoscopic endonasal transsphenoidal surgery: Experience with 50 patients. Journal of Neurosurgery 1997; 87:44-51.
11. Jho HD, Alfieri A. Endoscopic endonasal pituitary surgery: Evolution of surgical technique and equipment in 150 operations. Minimally Invasive Neurosurgery 2001; 44:1-12.
12. Kabil MS, Eby JB, Shahinian HK. Fully endoscopic endonasal vs. transseptal transsphenoidal pituitary surgery. Minimally Invasive Neurosurgery 2005; 48:348-354.
13. Kanaan IN. Minimally invasive approach to management of pituitary adenomas. Minimally Invasive Neurosurgery 2005; 48:169-174.
14. Cappabianca P, Cavallo LM, Colao A, De Caro MDB, Esposito F, et al. Endoscopic endonasal transsphenoidal approach: Outcome analysis of 100 consecutive procedures. Minimally Invasive Neurosurgery 2002; 45:193-200.
15. Yaniv E, Rappaport ZH. Endoscopic transseptal transsphenoidal surgery for pituitary tumors. Neurosurgery 1997; 40:944-946.
16. Rudnik A, Zawadski T, Wojtacha M, Bazowski P, Gamrot J. Endoscopic transnasal transsphenoidal treatment of pathology of the sellar region. Minimally Invasive Neurosurgery 2005; 48:101-107.
17. Kawamata T, Kamikawa S, Iseki H, Hori T. Flexible endoscope-assisted endonasal transsphenoidal surgery for pituitary tumors. Minimally Invasive Neurosurgery 2002; 45:208-210.
18. Cavallo LM, Briganti F, Cappabianca P, Maiuri F, Valente V, et al. Hemorrhagic vascular complications of Endoscopic transsphenoidal surgery. Minimally Invasive Neurosurgery 2004; 47:145-150.
19. Black PM, Zervas NT, Candia GL. Incidence and management of complications of transsphenoidal operation for pituitary adenomas. Neurosurgery 1987; 20:920-924.
20. Ciric I, Ragin A, Baumgartner C, Pierce D. Complications of transsphenoidal surgery: Results of a national survey, review of the literature and personal experience. Neurosurgery 1997; 40:225-237.
21. Laws ER. Vascular complications of transsphenoidal surgery. Pituitary 1999; 2:163-170.
22. Kassam A, Snyderman CH, Carrau RL, Gardner P, Mintz A. Endoneurosurgical hemostasis techniques: Lessons learned from 400 cases. Neurosurgical Focus 2005; 19(1):1-6.
23. Sabel M, Stummer W. Haemostasis in spine surgery. The use of local agents: Surgicel and Surgifoam. European Spine Journal 2004; 13(Suppl.1):97-101.
24. Dandy WE. Cerebral ventriculoscopy. Johns Hopkins Hospital Bulletin 1922; 33:189-190.
25. Cappabianca P, Briganti F, Cavallo LM, de Divitiis E. Pseudoaneurysm of the intracavernous carotid artery following endoscopic endonasal transsphenoidal surgery, treated by endovascular approach. Acta Neurochirurgica 2001; 143:65-96.
26. Stangerup SE, Dommerby H, Lau T. Hot-water irrigation as a treatment of posterior epistaxis. Rhinology 1996; 34:18-20.
1. Neurosurgeon Assistant Doctor of Neurosurgery Discipline at Escola Paulista de Medicina.
2. ENT Assistant Doctor of ENT Discipline at Escola Paulista de Medicina.
3. Neurosurgeon Doctor - Former president at Escola Paulista de Medicina.
4. Neurosurgeon Resident Doctor at Escola Paulista de Medicina.
Universidade Federal de São Paulo - Escola Paulista de Medicina - (Federal University - São Paulo).
Dr. Francisco de Assis Vaz Guimarães Filho
Address: - Rua Napoleão de Barros, 715, 6º andar, Secretaria da Disciplina de Neurocirurgia - Vila Clementino - São Paulo/SP - Brasil - CEP: 04024-002 - Fax: (11)5549.6834 - E-mail: vazguimaraes.neuro@gmail.com
This article was submitted to SGP (Sistema de Gestão de Publicações - Publication Management system) of R@IO on March 30th, 2007 and approved on August 21st, 2007 at 18:17:23.