INTRODUCTION AND REVISION OF LITERATUREThe obstructive sleep apnea syndrome (OSA) is a pathologic condition which implicates in serious negative repercussions to the individual´s health and functionality such, diurnal excessive somnolence (DES), cardiac arrhythmia, arterial hypertension, besides social and behavioral consequences. The high prevalence and wide spectrum of exposure imposes the medical treatment of this condition(1).
Among the existing practices to the OSA medical treatment, the positive pressure in the upper airways (CPAP) which is truthfully effective and, usually, the first choice method, the diets, the intra-oral orthodontic devices and surgery treatments which are indicated in special cases(2,3), stand out. The phonological myofunctional oral therapy may represent a new therapeutic option for snoring patients with or without OSA, as will be mentioned further ahead(4,5).
The positive pressure in the upper airways (CPAP), idealized by Sullivan et al.(6), is the continuous positive pressure medical treatment in the upper airways (UA) through a nasal or oronasal mask. This therapeutic modality is considered the most effective in cases of OSA carriers patients, mainly those who presents expressive drop of the oxygen saturation (SaO2), moderate OSA and severe OSA. Some limitations to its use are connected to the mask which may cause discomfort, rejection on the part of the partner, air leakage generating allergies and cutaneous irritations which occurs in mouth breathers patients, due to nasal obstruction, which may culminate with the low adhesion.
The loss of corporal weight through diets or surgery treatments is another therapeutic option. Ponderal reductions of 10% of corporal weight may lead to the reduction of up to 50% of the apnea/hypopnea index (AHI), and with 20% of corporal weigh loss, the patient may become asymptomatic. This fact is explained by the loss of adipose tissue in the whole body, including in the oropharyngeal region. However, the long term success rates are discouraging with the regaining of weight and reappearance or aggravation of the OSA(7).
The intra-oral devices, lingual retainers and jaw (mandible) positioners, are indicated to OSA carriers patients from moderate to slight and retrognathic OSA who are not above the ideal weight and have not severe oxyhemoglobin desaturation. Besides those counter-indications, patients with insufficient number of teeth to support the device, use of extensive dental prosthesis, periodontic problems, intense temporomandibular joint dysfunction (TMJ) and carriers of important anatomical alterations in the upper airways (UA), must not be treated with the intra-oral device for not reaching good results(8).
The surgery techniques vary from otorhinolaryngologic surgeries and maxillary functional orthopedic surgeries, which present variable results. The most common procedures reach between 40% and 50% of efficiency(9), and many times more than one techniques must be combined, at the same surgery time or in two separate times, so that the results may be more satisfactory(10).
The treatment modalities aforementioned described may act in palliative way, since they may not effectively treat the factor that precipitates the installation of the OSA or they are of difficult adhesion by the patients (high cost, long term difficult maintenance, etc.). Thus, in the pursuit of other therapeutic methods, it was raised the hypothesis of the phonoaudiological intervention in snoring patients with or without OSA through the myofunctional oral therapy, to bring benefits for these patients.
The myofunctional therapy consists, initially, of the necessity of being aware of the problem and correct it, the improvement of the body posture, the performance of the basic exercises and, finally, a reinforce period aiming at maintaining the new standards reached in the aforementioned stages. The exercises are divided in relaxing and breathing exercises, specific exercises to stimulate and adequate the functions of the stomatognathic and articulatory systems(11).
The contribution of the phonoaudiology in these cases is based on the fact that the apneic and snoring patients present a neuromuscular and/or structural exposure of its upper airways (UA), culminating in a significant reduction of the muscular tonus and increase of the resistance of the UA during sleep(12,13). It is also believed that the dilating force of the UA muscles is the only force responsible for counterbalance the forces which promotes the collapse, represented by the negative pharyngeal transmural pressure and for the weight of the structures which form the UA(14,15), fact that justify the rehabilitation of the orofacial and pharyngeal musculature of these individuals.
Therefore, the oral myofunctional therapy, directed to snoring patients with or without OSA, aims the posture adequacy, the sensibility and proprioception and the tonus and mobility of the orofacial and pharyngeal musculature. The structures prioritized in this work are those which may be related with the obstruction by the UA collapse during sleep: Floor of the oral cavity, tongue, especially the genioglossus muscle; mastication muscles, buccinator, masseter, lateral and medial pterygoid, digastric; soft palate and uvula; supra-hyoid and infra-hyoid muscles; pharyngeal musculature and the breathing, mastication and deglutition functions(4,5).
The objective of this study was to report the effectiveness of the oral myofunctional therapy in 2 patients with severe OSA from the analysis of the variables of the polysomnography (PSG) before and after the phonoaudiologic intervention with the reduction of the AHI, normalization or enhancement of the blood oxygenation of the sleep architecture as well as the evaluation of the punctuation in the Epworth Sleepiness Scale(ESE) and Snoring Score(SS).
CASES REPORT
Clinical Case 1Male patient, 37 years old, body mass index (BMI) 26,29 kg/m2 complaining about snoring, breathing stops during sleep, frequently awakenings, mood alterations, difficulties of concentration and memory deficit. In the polysomnography exam the patient presented AHI of 48.5% events per hour (e/h), average oxygen saturation (SaO2) of 92%, minimum of 79%, with T 90 (percentage time in which the SaO2 is placed below of 90%) of 5,9%. The patient presented micro-arousals (MA) index of 32/h, ESE=12 and SS=3. The SS is graded from 0 to 4, being 0=snoring absence, 1=resound (breathe heavily), 2=light snoring, 3=snoring that disturb the partner, 4=snoring that disturb the family (it surpasses the bedroom). In the otorhinolaryngological evaluation just a discrete increase of the inferior nasal shells was verified, and in the phonoaudiolological evaluation a crackle in the right TMJ, cheeks asymmetry with a bigger volume to the left, discrete reduction of cheeks, tongue and lips mobility and internal marks in the cheeks and tongue was observed.
From the diagnosis of severe OSA, the treatment with the nasal CPAP (continuous positive airway pressure) was indicated. However, the patient did not adapt himself and refused the treatment also for its cost. Thus, the patient was sent to the Phonoaudiologic service of the University Hospital of Brasília. The phonoaudiological intervention consisted in 16 sessions of myofunctional therapy performed by the same speech therapist when the patient was orientated to perform daily isometric exercises, aiming at increasing the muscular tonus; isotonic exercises, to improve the mobility, and isokinetic exercises, indicated to the relaxing and coordination specific for the oral cavity floor musculature, tongue, buccinator, masseter, lateral and medial pterygoid , digastric, soft palate and uvula; supra and infra hyoid muscles and pharyngeal musculature. The patient also received orientation about the importance of the nasal breathing. After the myofunctional therapy, a new polysomnography (PSG), phonoaudiologic evaluation, and ESE and SS application were carried out.
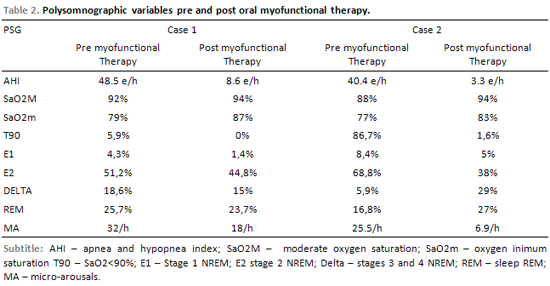
The patient reported, to the subjective evaluation, sleep enhancement, memory enhancement, and a better performance at work. According to the report, there was a snoring and respiratory arrests reduction during the sleep, although, the patient has not reported significant reduction of the snoring intensity, SS=2 (Table 1). In the control of the PSG, a reduction of the AHI (8.6/h); minimum SaO2 (87%) and T90 (0%) (Table 2) was verified. As for the sleep fragmentation, an 18/h reduction of the micro-arousals/hour index, was verified. In the ESE, the patient presented a reduction of 10 points in the punctuation (Table 1). It is valid to make reference to the BMC, factor considered predictive for the OSA, after treatment, which increases to 27.68 kg/m2 due to a ponderal gain of 4 kg. In the phonoaudiological evaluation a discrete reduction of the cheeks asymmetry and an improve of the orofacial structures tonus and mobility was verified in a subjective way, and crackles in the TMJ were not observed anymore, in spite of not being performed any exercises directed specifically to the TMJ.

Female patient, 55 years old, BMI 22,2 kg/m2, complaining about intense snoring, respiratory difficulty during sleep, frequent memory lapses and DES (diurnal excessive somnolence). The initial PSG demonstrated: AHI=40.4/h, SaO2M=88%, SaO2m=77%, T90=86.7%, MA=25.5/h. The applied subjective questionnaires made evident: ESE=13 and SS=3. Due to the non adaptation to the CPAP and to the intra-oral device, the patient was sent to the phonoaudiological evaluation and intervention, in the phonoaudiologic clinic of the University Hospital of Brasília. The otorhinolaryngological exam made evident a discrete nasal septum deviation, increase of the tongue base and a light retrognathism. In the phonoaudiological evaluation the patient presented a reduction of the cheek, tongue, lips and soft palate tonus and mobility, as well as, phonoarticulatory incoordination and nasal and superficial breathing.
The phonoaudiological intervention consisted in 16 myofunctional therapy sessions performed by the same speech therapist, when the inadequate and adequate standards of the correct posture and the movement of the phonoarticulatory organs had been approached aiming at obtaining the awareness of the alterations presented by the patients, and specific exercises, which should be performed daily for the patient, had been proposed. The exercises had been divided in isometric, isotonic and isokinetic. The patient also received orientation about the importance of the nasal breathing.
After the 16 weeks of myofunctional therapy, a new polysomnography (PSG), phonoaudiologic evaluation, and ESE and SS application was carried out. There was not BMI variation. The patient reduced the ESE punctuation to 7and the SS to 2 (Table 1). The comparison of the results of the first and second Polysomnographies demonstrate a clear improve of the studied variables. AHI 3.3/h, SaO2M 94%, SaO2m 83%, T90 1.6%, MD 6.9% (Table 2). In the subjective phonoaudiological evaluation an improvement of the orofacial structures tonus and mobility, as well as an improvement of the phonoarticulatory ccoordination was verified. Subjectively, the patient reported an improvement in the memory lapses and in the DES, which were important complaints before the treatment.
DISCUSSIONThe use of the orofacial motricity turned to snoring patients with or without OSA is still incipient, however, some authors demonstrated favorable results, as the results presented by Guimarães(3) and Pitta(4). There is a close relationship between the OSA´s physiopathology and the object of study of the orofacial motricity, specialty of the phonoaudiology, which are the structural and functional aspects of the orofacial and cervical regions, usually compromised in patients with OSA. However, this statement deserves corrections and needs more investigation aiming at proving the efficiency of the myofunctional therapy in this population.
It is valid to point out that the two patients who participated of this study were informed about the indication of the first chose treatment, the CPAP, and about the intra oral device, therapeutics already scientifically consolidated, but due to financial issues and non adaptation they opted for the execution of the oral myofunctional therapy, from the signing of a free and informal document.
In the cases studied, an expressive reduction of the AHI, which returned to values considered standards of normality, tendency or effective normalization of the oxygen saturation and a reduction of the micro-arousals index were verified, and subjectively, a reduction of the diurnal excessive somnolence and snoring, however there was not significant variation or improvement in the sleep architecture. The improvement of the respiratory variables objectively analyzed through the PSG suggests some degree of efficacy of the proposed oral myofunctional therapy. It is necessary to point out that the oral myofunctional therapy was applied as a mono therapy, that is, the patients did not perform other treatment concomitantly. nor presented changes in the quotidian activities which could compromise the obtained results.
The results pre and post oral myofunctional therapy corroborated with the hypothesis of the existence of a hypothony of the UA in patients with OSA, favoring the collapse of the oropharynx and obstruction of the aerial flux. The retrognathic profile of the patient of the case 2 configures one more risk factor to the OSA development, since it reduces the UA space and projects the tongue, in this case with an increased base, to a more posterior position. However, the myofunctional therapy did not have any interference in the change of the craniofacial profile of the patient, except the orofacial and pharyngeal musculature, which were exercised.
FINAL CONSIDERATIONSThe Phonoaudiology is a relatively new science of the health area, which has been expanding its therapeutic possibilities in order to reach areas until then unused. This is the inter relationship case between the Phonoaudiology and the Sleep Medicine, more specifically, the sleep respiratory disturbances.
This relationship backs to the fact that the structures involved in the obstructive respiratory disturbances, as the OSA and snoring, are neuromuscular units, in other words, the object of study and intervention of the Orofacial Motricity area.
Finally, the obtained results in this case study suggests that the oral myofunctional therapy may represent an alternative in the treatment of the severe OSA carriers patients who did not adhere to the CPAP, first choice treatment already consolidated in the scientific community. However, we conclude that is necessary to continue with this research increasing the number of studied cases and their follow-up in a longitudinal way.
BIBLIOGRAPHY1. America Sleep Disorders Association. The international classification of sleep disorders 1997, revised. Rochester MN: ASDA, 2001.
2. Chediak AD. Pathogenesis of obstructive sleep apnea. Respir Care. April 1998; vol.43 nº4. p.265-276.
3. Leiter JC. Analysis of pharyngeal resistence and genioglossal EMG activity using a model of orifice flow. J Appl Physiol. 1992; 73:576-583.
4. Guimarães K. Alterações no tecido mole de orofaringe em portadores de apnéia do sono obstrutiva. Jornal Brasileiro de Fonoaudiologia, 1999, Ano 1(1):69-75.
5. Pitta DBS. Avaliação da eficácia da intervenção fonoaudiológica - terapia miofuncional - em pacientes roncadores com e sem síndrome da apnéia obstrutiva do sono. Brasília, 2005, p.120. Dissertação de Mestrado - Faculdade de Medicina da Universidade de Brasília.
6. Sullivan et al.. Reversal of obstructive sleep apnea by continuous positive airway pressure applied through the nares. Lancet. 1981; 1:862-865.
7. Charuzi I, Ovnat A, Peiser J, Saltz H, Witzman S, Lavie P. The effect of surgical weight reduction in sleep apnea quality in obesity-related sleep apnea syndrome. Surgery, 1985, 95:535.
8. Shimidt-Nowara, Lowe et al. Oral appliances for the treatment of snoring and sleep apnea: a review. Sleep. 1995 Jul.; 18(6):501-10.
9. Riley, Powel e Guilleminault. Obstructive sleep apnea: a review of 306 consecutively, treat surgical patients. Otolaryngol. Head Neck Surg. 1993; 108(2)117-25.
10. Sher, Schechtman e Piccirillo. The efficacy or surgical modifications of the upper airway in adults with obstructive sleep apnea syndrome. Sleep. 1996; 19(2):156-77
11. Marquesan IQ. Motricidade oral: visão clínica do trabalho fonoaudiológico integrado com outras especialidades. 2ª ed. São Paulo: Pancast, 1999. p.24-81.
12. Ayappa I, e Rapoport DM. The upper airway in sleep: physiology of the pharynx. Sleep Med Rev, 2003, vol 7, nº.1, pp.9-33,
13. Mezzanote WS, Tangel DJ, White DP. Influence of sleep onset on upper airway muscle activity in apnea patients versus normal controls. Am. J. Respir. Crit. Care. Med. 1996; 153:1880-1887.
14. Schwab et al. Upper airway and soft tissue anatomy in normal subjects and patients with sleep-disordered breathing: significance of the lateral pharyngeal walls. Am. J. Respir. Crit. Care Med. 1995; 152(5pt 1):1673-1689.
15. Séries F. Upper airway muscles awake and sleep. Sleep Med Rev, 2002, vol. 6, nº.3, 229-242.
1. Master. Professor Fonoaudióloga Clinic.
2. PhD. Clinical Professor Fonoaudiólogo.
3. PhD. Otorhinolaryngologist.
4. PhD. Neurologist Sonologista.
5. Master. Psychologist.
6. PhD. Full Professor of Pulmonology at the University of Brasilia.
Institution: Sleep Laboratory of the University Hospital of the University of Brasilia, Brasilia/DF.
Danielle Silva and Barreto Pitta
Mailing address: SHIN IQ 06 - Conj 11 - House 06 - Brasilia/DF - CEP: 71520-110 - Phone: (61)8445-2184/3468-3853 - E-mail: danielle.pitta @ hotmail.com
This article was submitted in System Management Publications (SGP) by R@IO on 22 October 2006. Cod. 175. Article accepted on February 26, 2007.