INTRODUCTIONThe Necrotizing Fasciitis (NF) is a bacterial disease, quickly progressive, characterized by an extensive necrosis of skin, subcutaneous tissue, fascias and muscle (1). Firstly described by Jones in the American Civil War in the Ninth Century as a bacterial complication in injuries from firearm, it is a potentially fatal disease (2).
The Necrotizing Fasciitis prevails in the adult population compared to children and some systemic disorders and local factors, such as alcoholism, diabetes, intravenous drug use, immunosuppression, dental alterations, slight traumas, folliculites are associated with this disease (3,4).
The most commonly affected locations are the abdominal wall, the extremities, pelvis and thoracic wall and it's less common in the head and neck region (1).
In the initial stage, the infection is located in the superficial fascia. The evolution occurs with small and medium blood vessels thrombosis and in this phase the skin becomes erythematosus and edematous, develops vesicles and presents with an aspect of "orange peel". Due to the inadequate perfusion the skin then becomes ischemic and necrotic. The muscular involvement is rare and when affected it suggests Clostridium infection and is named Clostridial Myonecrosis (5).
The pathogens involved in the necrotizing fasciitis are heterogeneous and comprise aerobic and anaerobic bacteria. The most frequently isolated microorganisms are the Streptococcus pyogenes (group A) and Staphylococcus aureus, which produce toxins and enzymes that activate colagenases and hyaluronidases and lead to subcutaneous tissues necrosis. The anaerobic bacteria such as Clostridium, Bacterioids and Fusobacteria are responsible for the tissues gas and fermentation production (1).
The anatomopathological exam is the most precise diagnostic method for the early disease identification. The contrast computerized tomography is important to check the disease extension, the relationship with anatomic structures and the infection primary site location. This disease main complications are mediastinitis, pericartitis, septic shock, respiratory obstruction, arterial erosion and jugular vein thrombosis.
The early and aggressive surgical debridement, as well as the wide spectrum antibiotic therapy and hemodynamic support are essential for the treatment. When the surgical procedure is carried out before 48 hours as from the diagnosis, the survival rate is higher than 75% (6).
CASE REPORTThe 2-month-old, male sex, white patient was brought to the Emergency Room of the Base Hospital / FAMERP with a history of cervical convexity to the right associated to irritability and (non-verified) fever with 1 day of evolution. The infant's mother denied that he had presented with an URI episode, trauma or any alteration. She reported the child had been born of Cesarian birth with 39 weeks and 5 days, agar 9/10, weight 2840g. He was fed of exclusive breast-milk, the vaccinations were up to date and he was periodically followed up by the pediatrician.
Upon physical exam the child presented with good general state, eupneic, colored, hydrated and febrile (T = 38.5oC). Upon rhinoscopy, oroscopy and otoscopy he didn't have any alteration. In the cervical inspection and palpation the cervical convexity was confirmed in areas I, II, III and IV to the right, of approx. 5 x 5 cm of diameter, with poorly defined limits, hyperemia, pain and local heat. The facial mimicry was preserved.
Before such picture the diagnostic hypothesis of deep cervical abscess was made and the child was interned with intravenous antibiotic therapy: Cephalotin (100mg/Kg/day) and Amikacin (15mg/Kg/day), associated to hormonal anti-inflammatory: Dexametasone (0.15mg/Kg/dosage) and with analgesics (Dipirone). We also requested laboratorial exams that revealed relative and absolute lymphopenia with 5.900 leucocytes (VN > 11,000), 68% were segmented and 22% of typical lymphocytes, and elevation of reactive C protein (RCP) with value of 20mg/dl (VN = 0 to 1 mg/dl).
On the 2nd day of internment (DI), the patient was submitted to surgical draining with release of purulent secretion (sent for culture) and debridement of devitalized muscular areas (sent for anatomopathological evaluation).
On the 3rd DI the patient evolved with skin suffering signs in operative injury (Picture 1) and we opted in the Pediatrics Service for the exchange of Cephalotin for Clyndamicin, surgical debridement of the devitalized tissue areas, whose anatomopathological evaluation revealed fibro-adipous and muscular tissue with an extensive necrosis area, compatible with necrotizing fasciitis. Before such picture, the patient was transferred to the Pediatric ICU, where he remained for 33 days.
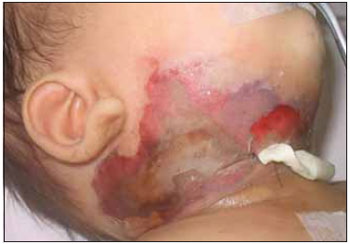
Picture 1. Cervical region with skin involvement signs.
Within this period, four more surgical debridements were performed (7th, 9th, 14h and 16th DI) and the operative injury remained opened with exposure of the right cervical region musculature (Picture 2).
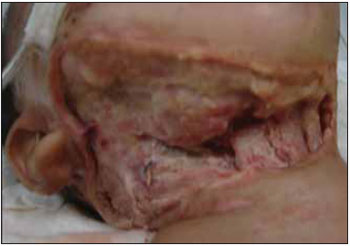
Picture 2. Operative injury after surgical debridement with exposure of cervical structures.
On the 4th DI the Pediatrics Service guided the antibiotic therapy change for Vancomycin, Cephepime used for 22 days and Metronidazol for 12 days (based on the Streptococcus viridans and Pseudomonas aeruginosa in the cervical secretion drained on the 2nd DI).
We washed the injury everyday with physiological saline 0.9% and cholheridine degermant and curatives with absorbing plates (Hidrogel®). For a better evolution of the healing the patient was also submitted to hyperbaric chamber sessions.
As complications during the interment, the child presented with right facial nerve paralysis of the marginal branch (1st PO of cervical abscess draining), he needed blood transfusions due to the hematocrit fall after the debridements and two Pediatric Surgery interventions for correction of the umbilical hernia.
The infant was discharged from hospital after 42 interment days, with the cervical injury in healing process for second intention (Picture 3), daily curatives with physiological saline instruction and remains in service follow-up without great functional or aesthetic changes (Picture 4).
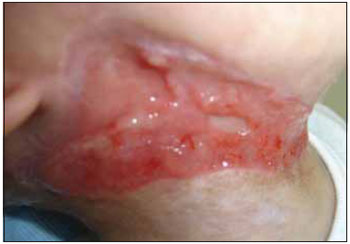
Picture 3. Operative injury in granulation process.
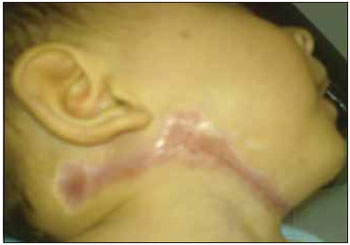
Picture 4. Final aspect of the operative injury second intention healing.
The Necrotizing Fasciitis is more frequent in the adult population then in children. According to Ricalde et al (5), the most notorious difference between adults and children is that almost all children with necrotizing fasciitis are fully healthy. The author found 11 cervico-facial NF cases in people younger than 16 years old described in the English literature and all were previously healthy, as in the case presented.
The head and neck region is an uncommon affection place. When this region is affected, the infection is more frequent in the frontal cervical region (60% of the cases), followed by the face, with affection around 17% (1). The patient in our report presented infectious signs across the frontal and right side cervical region.
In spite the most frequent pathogens involved in the necrotizing fasciitis are the Streptococcus pyogenes (group A) and the Staphylococcus aureus, Lang et al (7) reported a case of necrotizing fasciitis involving the head and neck of a 5-month-old infant in whom the Group B Streptococcus was isolated. In this work the authors considered the prematurity to be a risk factor and suggested a nosocomial origin for the NF caused by this microorganism.
In the case described the Streptococcus viridans was isolated and in our bibliographic review we found no case in which this bacterium was so far isolated.
The anatomopathological exam confirmed the disease. The computerized tomography was not carried out in our patient because the physical exam didn't show any extension or complication of the disease and the patient had been presenting with clinical and laboratorial significant improvement.
The surgical debridement performed was early and aggressive, as well as the large spectrum antibiotic therapy, as recommended in the literature.
The secondary therapy with hyperbaric oxygen remains controversial. Mohammed et al (8) observed that it may be beneficial in the initial phase of the Clostridial Myonecrosis; however, this type of treatment may be harmful because the aerobic bacteria are significant components in the soft tissues infection.
In our report the infant's operative injury was treated with alginate-based curatives, which absorb the exudate and maintain the injury site moist and stimulate the autolytic debridement. Simultaneously, the patient was treated with hyperbaric chamber. The operative injury was healed by second intention and the infant evolved with an excellent result.
CONCLUSIONThe Necrotizing Fasciitis (NF) is a bacterial disease, quickly progressive, characterized by an extensive superficial fascia necrosis, subcutaneous tissue, fascias and muscle and skin (1).
In children it's an uncommon pathology and the head and neck region affection is not frequent. The early detection and aggressive surgical debridement are essential for these patient's therapeutic success.
As a secondary therapy the utilization of large spectrum antibiotic therapy and hemodynamic support are indispensable.
BIBLIOGRAPHICAL REFERENCES1. Berlucchi M, Galtelli C, Nassif N. et al. Cervical necrotizing fasciitis with mediastinitis: a rare occurrence in pediatric age, American Journal of Otolaryngology. 2007, 28:18-21.
2. Jones J. Editor, Investigation upon the nature, cause, and treatment of hospital gangrene as it prevailed in the Confederate Armies 1861-1865, Surgical Memories of the war of Rebellion US Sanitary Comission, New York (1871).
3. Cavel O, Gil Z, Khafif A. et al, Necrotizing Fasciitis of the Skull Base and neck in a pacient with AIDS and Non- Hodgking's Lymphoma. Skull Base. 2006, 16:201-206.
4. Hanna BC, Delap TG, Scott K. et al. Surgical debridament of craniocervical necrotizing fasciitis: the window of opportunity. The Journal of Laryngology and Otology. 2006, 120:702-704.
5.Ricalde P, Engroff SL, Jansisyanont P. et al, Pediatric necrotizing fasciitis complicating thir molar extraction: report of a case. Int. J. Oral Maxillofac Surg. 2004, 33:411-414.
6.Moss RL, Musemeche CA, Kosloske AM. Necrotizing fasciitis in children: prompt recognition and aggressive therapy improve survival. J Padiatric Surg. 1996, 31:1142-1146.
7. Lang ME, Vaundry W, Robinson JL. Case report and Literature Review of late- Onset Group B Streptococcal Disease manifesting as necrotizing Fasciitis in Preterm Infants: Is this a New Syndrome? Clinical Infectious Diseases. 2003, 37:132-135.
8. Mohammedi I, Ceruse P, Duperret S. et al. Cervical necrotizing fasciitis: 10 years' experience at a single institution. Intensive Care Med. 1999, 25:829-834.
1. Resident Doctor in the 3rd year of the Otorhinolaryngology and Head and Neck Surgery Department - Base Hospital / FAMERP.
2. Otorhinolaryngologist Doctor. Otorhinolaryngologist of Hospital São Joaquim - UNIMED of Franca and Santa Casa de Franca / SP.
3. Otorhinolaryngologist. Otorhinolaryngologist Doctor.
4. Otorhinolaryngologist. Responsible for the Service of Otorhinopediatrics of the Otorhinolaryngology and Head and Neck Surgery Department - Base Hospital / FAMERP.
5. Otorhinolaryngologist. Responsible for the Service of Rhinology of the Otorhinolaryngology and Head and Neck Surgery Department - Base Hospital / FAMERP.
Institution: Faculdade de Medicina São José do Rio Preto - FAMERP / Hospital de Base. São José do Rio Preto / SP - Brazil.
Mail address:
Renata Rennó Schiavetto
Rua Joaquim Manoel Pires, 273, Apto. 13 - Bairro: Pinheiros
São José do Rio Preto / SP - Brazil - Zip code: 15091-210
Phone: (+55 17) 3229-3131 - Fax: (+55 17) 3201-5000
E-mail: renata.rs@bol.com.br
Article received on November 25, 2007.
Approved on June 15, 2008.