INTRODUCTIONAnterior approaches to cervical spine have been used routinely by orthopedists and neurosurgeons in therapies of degenerative or traumatic diseases of cervical spine (1). However, complications might occur during this procedure, though it requires dissection next to important organs and nerves (2-4). Dysphagia and dysphonia are conditions commonly associated to it (5-14). Due to the increase of the number of this surgery, the iatrogenic paralysis of vocal fold has been more frequently associated to the diskectomy and/or anterior cervical corpectomy than the thyreoidectomy (15), because of section, division, stretching or compression of the recurrent laryngeal nerve (1,16-19). Iatrogenic dysphagia has been associated to the lateral retraction to which larynx, pharynx and esophagus are submitted to make the approach to the cervical spine possible (20-21).
Even deglutition and voice disorders are related to this surgical procedure, understanding the nature and the etiology of symptoms is not very clear and complaints are not well accepted by health professionals and also hardly mentioned by patients (7,9,10,13,22).
The target of this study is to establish a relation between cervical spine surgery with right anterior approach and the presence of signs and symptoms of dysphagia and dysphonia, at three distinct moments: pre-operative, immediate postoperative and late postoperative period, after the speech therapy interview.
PATIENTS AND METHODSThirty patients submitted to right anterior approach to the cervical spine between February, 1995 and July, 2004, according to records from Neurosurgery Service of the Hospital Universitário Cajuru (HUC)/PUCPR, were called and agreed to participate in the research, approved for the Committee and Ethics in Research - PUCPR and registered in the CEP under number 315, signing the "Free and Clear Consent Term". Form these, thirteen were male (43%) and seventeen were female (57%). The average age was 54.5 years. The minimum age was 23 years and the maximum was 83 years. All the patients were operated by the same neurosurgeon, who chose the right approach due to personal preference and easily handled ability.
Surgical procedures consisted of performing diskectomy followed by arthrodesis in 14 patients (47%) and corpectomy, diskectomy and arthrodesis in 16 patients (53%).
Twenty-nine patients (97%) received iliac bone graft (removed from right anterosuperior iliac crest) and one patient (3%) received insertion of a prosthesis of tricalcium phosphate (Biosorb). After grafting procedure, patients were submitted to internal fixation of it through plates of Caspar and titanium screws.
From the twenty-nine patients submitted to the diskectomy, nine of them (31%) had two approached levels, sixteen (55%) had two ones, and four (14%) had three approached levels. Level C3-C4 was surgically approached in 3 patients, level C4-C5 in 15 patients, level C5-C6 in 21 patients and level C7-T1 in one patient. In one particular patient it was necessary re-operation due to formation of bruises in the surgical area.
The research was based on a retrospective study, and analysis of the medical report of the patients, on application of a questionnaire based on phonation and deglutition questions and performance of a phonoaudiological evaluation of the voice and deglutition by a speech doctor who participated in the study. The collection of data was performed between June and September, 2004.
The clinical evaluation of the voice was based on the proposal by Behlau and Pontes(23), taking into consideration the following parameters: maximum phonation time (MPT), relation s/z, vocal pitch, vocal intensity, breathing and pneumo-phono-articulation coordination. The perceiving evaluation of the voice was performed with the use of RASAT scale(24).
For the evaluation of the deglutition it was used, as reference, the protocol by Furkim and Silva(25), who suggest an indirect (with no food) and direct (with food) evaluations. In the former, aspects as strength, mobility and coordination of organs of deglutition process and others are analyzed. The functional evaluation of the deglutition (direct) was performed with the use of three consistencies: liquid (water), pasty (apple pulp) and solid (biscuit), verifying aspects such as: capitation of food, labial closing, oral restraint, preparation and transport of food, deglutition reflex, laryngeal rise, and presence of indicative clinical signals of laryngotracheal aspiration.
It made part of the research patients submitted to anterior approach to the cervical spine, for treating disc hernia, degenerative or traumatic diseases; patients operated in the Neurosurgery Service at HUC for one of the authors (LRA), from February, 1995 to July, 2004 aging over 18 years; patients who signed the free and clear consent term. It did not make part of the research, patients complaining of dysphagia and dysphonia; with sequelae from neurological diseases and patient who did not make part of the interview and phonoaudiological evaluation in the clinic.
RESULTSPatients were asked before complaints related to voice and deglutition at three distinct moments: in the pre-operative, postoperative and at the moment of the phonoaudiological interview (Table 1).
From the application of Wilcoxon's test, at the level of significance equivalent to
a = 0.05 (5%), one can affirm that there is a significant difference between complaints before and after surgery, and that those are related to the surgical procedure. It can also be affirmed that there is a significant reduction between complaints presented by patients after surgery and at the moment of the interview, what means, those complaints tend to reduce the time of surgery.
Based on the perception of the problem by patients, and using the system of classification by Bazaz et al.(13) as a reference, grade of discomfort regarding complaints were considered "mild" for occasional complaints (deglutition and/or voice) and with no restriction to any type of food and to the form of feeding; "moderate", when the difficulties were more often and required changes regarding eating habits and possibilities of communication, with difficulty for specific foods (bread or meat) and "severe", when the difficulties caused impact on quality of life and eating pleasure, which were tested during each eating period, and requiring from patients some changes regarding feeding manner and possibilities of communication (Table 2).

The presence of persistent complaints when swallowing made symptomatic patients use strategies to make their feeding easy such as: avoiding bread and hard meats, eating more slowly, alternating solids and liquids, chewing more before swallowing, cutting food in small pieces and spending more time on meals.
Symptoms started during postoperative period for 26 patients; from 30 to 60 days after surgery for one patient and 60 days after surgery for another patient.
Out of these 28 patients with complaints in postoperative period, thirteen of them did not have any symptoms and 15 remained symptomatic. For the first group of patients, complaints lasted up to one week for six patients; between two and four weeks for two patients; between one and three months for four patients and between six months and one year for one patient. For the group of patients who remained symptomatic until the moment of the interview, 14 of them presented signs and symptoms of dysphonia and/or dysphagia for more than fifteen months.
Gathering complaints regarding dysphagia and dysphonia in the postoperative period and at the moment of the interview, the following results were obtained (Table 3).
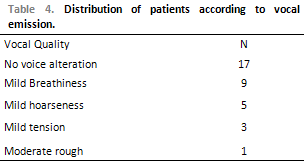
Regarding clinical evaluation of the voice, two patients presented maximum phonation time (MPT) in high level and eighteen patients presented reduced MPT. The relation s/z <1.1 was found in four patients, indicating constriction of the vocal folds to phonation; seventeen patients presented s/z between 1.0 and 1.1 showing balance between breathing and phonation, and nine patients presented numbers >1.1 indicating incorrect closure between vocal folds at the moment of phonation. Parameters such as vocal pitch, vocal intensity and breathing were adjusted in twenty-eight patients (93%). Five patients presented pneumo-phono-articulation disorientation, characterized by pauses and frequent air recharges in the speech. The vocal quality, modified in 13 patients (43%), was distributed in the following form (Table 4).
Mobility evaluation and the power of the phonoarticulatory organs were suitable in 100% of patients. The results from functional evaluation of the deglutition (Table 5) indicate alterations on pharyngeal phase of deglutition.
DISCUSSIONDysphagia incidence as a consequence of the right anterior approach has varied, according to literature, between 2.1% (26) and 60% (12). In the same way, dysphonia incidence has varied between 1.2% (27) and 51% (12).
The possible causes of dysphagia after surgery are: hypopharynx perforation and cervical esophagus (6,10,28), Tracheoesophageal fistula (9), hematoma and oedema (4,5,10,13), postoperative infection (5,10), surgical scar (4), displacement of bone graft, plates and screws (3,4,10,13), denervation on pharyngeal plexus (13,29), injury of the recurrent laryngeal nerve (4,13), injury of the superior laryngeal nerve (17,29), injury of the hypoglossal nerve (3,30) and pharyngeal and glossal nerve (8). Dysphonia has been associated to vocal fold paralysis in result of injury of the recurrent laryngeal nerve (1,3,9,10,16,18,29), injury of the superior laryngeal nerve (17,29,32), injury of the pharynx branches of the vagus nerve (9,29), oedema of pharynx and larynx tissues (16,17) and postoperative infection (5).
The signs and symptoms of deglutition disorders most commonly related to postoperative period of the cervical spine surgery are: discomfort when swallowing (26), difficulty for swallowing liquids and solids (4,6,10-12), difficulty in swallowing saliva (6), pain when swallowing (6,4,12,28), cough after it (6,10,18), aspiration (8-10,18), sensation of food stopped in the throat (4,10,12), reduced laryngeal rise (8,9), incomplete opening of the superior esophageal sphincter (8,10), difficulty in swallowing pills (11), reduction of propulsory power of the tongue (8), and others.
Yet, signs and symptoms of voice disorders are: hoarseness (3,8,10,12,17,18), vocal fatigue and breathing (9,10), difficulty in singing (10,11), pain when talking (12), difficulty in changing spitch (11), weak voice and reduction of vocal intensity (9).
In this study, the incidence of symptoms of dysphagia in the postoperative period was 93.3% and of symptoms of dysphonia was 43.3%, showing higher values than the ones found in most of other studies. It can be thought that the high incidence of dysphagia and dysphonia present in this study is due to the fact that patients, who participated in the interview and phonoaudiological evaluation, did it because they had complaints or even showed complaints related to deglutition and/or phonation. This fact might not express the real incidence of phonoaudiological alterations noticed in the postoperative period of anterior approach to cervical spine. Other studies, more patients and CT evaluations are necessary.
The most common symptoms mentioned in immediate postoperative period were: sensation of food stopped in the throat, difficulty in swallowing solids, pain when swallowing and hoarseness. At the moment of the interview the complaints were: sensation of food stopped in the throat, difficulty in swallowing solids, hoarseness and cough or choking after swallowing.
To some authors, the surgical approach at the right is understood as a risky factor for dysphagia and postoperative dysphonia (1,3,16,29). To others (14,27), there is no positive association between the approached side and the incidence symptoms, being the experience of the surgeon the decisive factor.
Surgical approach of multiple levels tends to result in bigger number of cases of dysphagia than the surgical boarding of a level only, since the access the multiple levels requires a more extensive manipulation and retraction of the organs, tissues and nerves and more surgeries (8,13). Other risky factors as sex (11,13), age (14), boarding to the inferior cervical spine (13), presence of previous history of hoarseness and dysphagia (12) and the necessity of surgical revision (3,8,12,2), are mentioned in literature.
In this study, due to the size of the sample, it was not possible to establish risky factors with significant statistics.
Failure of deglutition and voice are commonly associated to the initial postoperative period (13) and, generally, are considered transitory (9). The symptoms that persist for up to 48 hours are suggestive of oedema of the anatomical compartments, what favors the reduction of the pharynx contraction and stases in valecule and pear-shaped breasts, limited closing of the ESE, reduction of the movement of epiglottis and the larynges rise. However, the symptoms that persist beyond this period, have been related to the injuries of the involved organs, as surgical scar, hematoma, esofágica perforation and injury of the X skull nerve (5,9).
However, the beginning of the dysphonia and dysphagia symptoms can delay and not be related to postoperative the immediate one (4,6). This indicates the necessity of monitoring of the patients for a bigger period time, as for the symptoms of dysphagia and dysphonia, specialized professional advice and treatment for the joined alterations. The symptoms can, also, have longer duration (in some cases), or can even become permanent, leading to a chronic picture (11,16,29), what has been verified in this research.
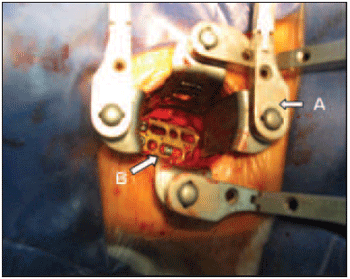
Figure 1. Afastadores medial and lateral, Caspar (A). Fixing the bone graft and plate with screws, titâneo (B).
The signs and symptoms of dysphalgia which are present in the moment of the speech therapy interview were considered mild (in higher proportion) or moderate (in lower proportion), which does not interfere significantly in the life quality of the patients. They seem to be used to the reminiscent difficulties, once most of the patients mentioned that they do not feel lack of eating pleasures neither of their favorite food. The modifications performed by such patients seem to compensate such difficulties. On the other hand, the complaints made on the immediate post-surgical phase, which were classified as severe, moderate or mild (in less proportion) significantly affect the well-being sensation and the recovery of patients, a fact that is mentioned in the literature (12).
The absence of alterations concerning mobility and power of orofacial organs and deglutition alterations which were verified in the functional deglutition evaluation refers to the pharingeous phase of deglutition. Such findings agree with Buchholz's article (7), who did not find evidence of alterations in the oral phase of deglutition but did so in the pharingeous phase.
The concern with the paralysis of decurrent vocal fold of injury of the recurrent laryngeal nerve during the surgery of cervical spine with previous access has been widely argued in literature (1,2,14,16-19,27,29). However, other studies show one high incidence of dysphagia as consequence of this surgical procedure (6,12). For Bazaz et al. (13), the postoperative dysphagia is one of the consequences of the surgery of argued cervical spine less.
Some authors (4,7,9-12,18,22) point out the fact that the dysphagia and the dysphonia, as consequence of the surgery of cervical spine with previous access, has been sub-diagnosised. The etiology of these complications clearly was not elucidated and the patients, rarely, are indicated for otorrinolaringologic and phonoaudioligic evaluation (3,4,10,12). At the same time in which voice and deglutition failures have important functional and legal implications, little attention has been given to it and little research has been lead with intention to decide these problems; the patients would have to receive daily pre-surgical and post-surgical advice (7,8-10,12).
CONCLUSIONSThe dysphagia incidence of symptoms and dysphonia in this study was of 93% and 43%, respectively, for the period of the postoperative one. At the moment of the interview, the incidence was of 40% and 20%, respectively.
Even if the alterations diminish some time after the surgery, many patients can remain symptomatic for a long period and, eventually, not present spontaneous remission of the symptoms, requiring daily post-surgical advice and otorrinolaryongologic and phonoaudiologic guidance for treatment of the joined alterations.
In this study, the dysphagic complaints had been more frequent than the dysphonic ones, as much in postoperative the immediate one as in postoperative the delayed one, what reinforces the necessity of higher studies on the frequency, severity and etiology of this complication, and a higher inquiry on the presence of these complaints among the patients, since they affect the sensation of well-being and the recovery of the patients in the postoperative one and require of the same ones, modifications of its alimentary habits in the long run.
It is believed that the results presented and discussed in this study can contribute to maximize the interest of surgeons and speech therapists in terms of the decurrent dysphagia and dysphonia of the surgical procedure which has been covered. Other studies, especially prospective ones, with evaluations before and after the surgery, became necessary. The understanding of the physiological mechanisms that result in these pictures is essential for the surgical and/or therapeutical treatment of the voice and deglutition, that must be initiated as fast as possible and to have multidisciplinary approach.
BIBLIOGRAPHY1. Ebraheim NA, Lu J, Skie M, Heck BE, Yeasting RA. Vulnerability of the Recurrent Laryngeal Nerve in the Anterior Approach to the Lower Cervical Spine. Spine 1997;22(22):2664-2267.
2. Weisberg NK, Spengler DM, Netterville JL. Stretch-induced Nerve Injury as a Cause of Paralysis Secondary to the Anterior Cervical Approach. Otolaryngol Head Neck Surg 1997;116(3):317-324.
3. Brislin BT, Hilibrand, AS. Avoidance of Complications in Anterior Cervical Revision Surgery. Current Opinion in Orthopaedics 2001;12(3):257-264.
4. Vanderveldt HS, Young MF. The Evaluation of Dysphagia after Anterior Cervical Spine Surgery: a Case Report. Dysphagia 2003;18:301-304.
5. Welsh JJ, Welsh LW, Chinnici JC. Dysphagia due to Cervical Spine Surgery. Ann Otol Rhinol Laryngol 1987;96:112-115.
6. Stewart M, Johnston RA, Stewart I, Wilson JA. Swallowing Performance Following Anterior Cervical Spine Surgery. British Journal of Neurosurgery 1995;9:605-609.
7. Buchholz DW. Dysphagia Following Anterior Cervical Spine Surgery. Dysphagia 1997;12:9-10.
8. Martin RE, Neary MA, Diamant NE. Dysphagia following Anterior Cervical Spine Surgery. Dysphagia 1997;12:2-8.
9. Daniels SK, Mahoney MC, Lyons GD. Persistent Dysphagia and Dysphonia Following Cervical Spine Surgery. ENT - Ear, Nose & Throat Journal 1998;77(6):470-475.
10. Winslow CP, Meyers AD. Otolaryngologic Complications of the Anterior Approach to the Cervical Spine. American Journal of Otolaryngology 1999; vol. 20(1):16-27.
11. Yue W, Brodner W, Highland TR. Persistent Swallowing and Voice Problems after Anterior Cervical Discectomy and Fusion with Allograft and Plating: a 5 to 11 year follow-up study. European Spine Journal, 2004. Disponível em: www.springerlink.com. Acesso em 23/03/05.
12. Winslow CP, Winslow TJ, Wax MK. Dysphonia and Dysphagia Following the Anterior Approach to the Cervical Spine. Archives of Otolaryngology - Head & Neck Surgery 2001;127(1):51-55.
13. Bazaz R, Lee MJ, Yoo JU. Incidence of Dysphagia after Anterior Cervical Spine Surgery. Spine 2002;27(22):2453-2458.
14. Baron EM, Soliman AMS, Simpson L, Gaughan JP, Young WF. Dysphagia, Hoarseness, and Unilateral True Vocal Fold Motion Impairment following Anterior Cervical Diskectomy and Fusion. Ann Otol Rhinol Laryngol 2003;112(11):921.
15. Benninger MS, Gillen JB, Altman JS. Changing Etiology of Vocal Fold Immobility. The Laryngoscope 1998;108:1346-1350.
16. Heeneman H. Vocal cord paralysis following approaches do the anterior cervical spine. Laryngoscope 1973; vol. 83:17-21.
17. Bulger RF, Rejowski JE, Beatty RA. Vocal Fold Paralysis associated with Anterior Cervical Fusion: considerations for Prevention and treatment. J. Neurosurg 1985;62:657- 661.
18. Morpeth JF, Williams, MF. Vocal Fold Paralysis after Anterior Cervical Diskectomy and Fusion. Laryngoscope 2000;110(1):43-46.
19. David WS, Petrozza PH. On the Incidence, Cause, and Prevention of Recurrent Laryngeal Nerve Palsies during Anterior Cervical Spine Surgery. Journal of Neurosurgical Anesthesiology 2001;13:180-181.
20. Buchholz DW. Neurologic Disorders of Swallowing. Groher ME. Dysphagia: Diagnosis and Management. 3ª ed. Boston: Butterworth-Heinemann, 1997:37-62.
21. Santini CS. Disfagia Neurogênica. Furkim, A.M.; Santini, C.S. Disfagias Orofaríngeas. São Paulo: Pró-Fono, 1999:19-34.
22. Edwards II CC, Kapitskaya Y, Cha C, et al. Accurate Identification of Adverse Outcomes after Cervical Spine Surgery. Journal of Bone and Joint Surgery 2004;86(2):251-257.
23. Behlau M, Pontes P. Avaliação e Tratamento das Disfonias. São Paulo: Editora Lovise, 1995.
24. Pinho SMR, Pontes P. Escala de Avaliação Perceptiva da Fonte Glótica. Jornal do Conselho Federal de Fonoaudiologia 2002;15(out.nov.dez):14-15.
25. Furkim AM, Silva RG. Programas de Reabilitação em Disfagia Neurogênica. São Paulo: Frôntis Editorial, 1999.
26. Clements DH, O´Leary PF. Anterior Cervical Discectomy and Fusion. Spine 1990;15(10):1023-1025.
27. Beutler WJ, Sweeney CA, Connoly, PJ. Recurrent Laryngeal Nerve Injury with Anterior Cervical Spine Surgery: Risk with Laterality of Surgical Approach. Spine 2001;26(12):1337-1342.
28. Gaudinez RF, English GM, Gebhard JS, Brugman JL, Donaldson DH, Brown CW. Esophageal Perforations After Anterior Cervical Surgery. Journal of Spinal Disorders 2000;13(1):77-84.
29. Netterville JL, .Koriwchak MJ, Winkle M, Courey MS, Ossof, RH. Vocal Fold Paralysis Following the Anterior Approach to the Cervical Spine. Ann Otol Rhinol Laryngol 1996;105:85-91.
30. Sengupta DK, Grevitt MP, Mehdidan SMH. Hypoglossal nerve injury as a complication of Anterior Surgery to the Upper Cervical Spine. Eur Spine J 1999;8:78-80.
1. Master in Communication Disorder by UTP (Speech doctor at Hospital Universitário Cajuru - PUCPR; Teacher in the Phonoaudiology course at PUCPR)
2. PhD by UFPR (ENT doctor and Endoscopyst; Teacher in the Phonoaudiology course at Universidade Tuiuti - Paraná)
3. PhD (Head of Neurosurgery Service at Hospital Universitário Cajuru - PUCPR; Teacher in the Medical School at PUCPR)
Universidade Tuiuti do Paraná Pontifícia Universidade Católica do Paraná
Beatriz Bornschein Alves de Souza
Address: Rua João Fernandes França, 123 - sobrado 02 Atuba Curitiba/PR - 82630-080
This article was submitted to SGP - Sistema de Gestão de Publicações (Publication Management System) from RAIO on July 11, 2006 and was approved on September 27, 2006 01:12:49.