INTRODUCTIONCyanoacrylate is a generic term which refers to substances such as 2-cyano-butil-acrylate or octil-2-cyanoacrylate, which is also known as dermabond
®. Sometimes they are called instantaneous adhesives. They are substances which have been discovered during the Second World War. In the liquid form, such substances consist of monometers of molecules of cyanoacrylates with the composition (C
5H
5NO
2) CH
2=C(CN)COOCH
3 and, in the presence of water, more specifically ions of hydrogen, they rapidly suffer a polymerization process forming an acrylic resin. Other important characteristic of this group of substances is its ability to solidify in less than one minute in the presence of water, which is different from other glues. The cyanoacrylates are better used in non porous materials and which contain, at least, traces of water(6). Their use in human body tissues is still stucy object in several areas both referring to use effectiveness and referring to risks and complications of their use.
Several Surgeons have been using cyanoacrylates in several medicine areas, especially in endoscopic, neurosurgical, aesthetic, orthopedic and otorhinolaryngological procedures. Several articles have been published involving its use. Its clinical and surgical use happened very fast once its adhesive properties have been verified by COOVER em 1959(1,2). We have demonstrated that the use of these substances advances fast in medicine, and it is considered essential in surgical areas. The complications due to cyanoacrylates have not been frequently verified in the clinical practice. However, there are embolic and endoscopic complications related in literature(4,5). The bactericide power of acrylates which dispenses the need to sterilize such substances(3) is pointed out.
Studies on animals demonstrated that cyanoacrylates have been considered effective in bone fixation(8), which has also been reported both in animals and humans(7). Based on these studies, we have observed the effectiveness of such substances on bone tissue adherence. Studies involving the use of prosthesis are rare and there is need to better evaluate its adhesive power on materials used on prosthesis manufacturing.
Besides the bactericide power which has been previously mentioned, the cyanoacrylates have other properties. There are many different kinds of molecules in the cyanoacrylate group which bring different physical and chemical properties according to the molecule's composition and conformation. Among the cyanoacrylates we can mention etil-2-cyanoacrylate (Super-bonder
®) and the metal-2-cyanoacrylate, which are short-chain, and the 2-cyanobutilacrylate (histoacryl
®), octilcyanoacrylate, isobutilcyanoacrylate e o fluoroalkilcyanoacrylate, which are long-chain. The long-chain cyanoacrylates are less toxic than the short-chain ones.
The cyanoacrylates have been adopted in many different uses within the otorhinolaryngology and head and neck surgery. However, they are still studied in terms of such uses' efficiency and of finding new uses for them. Among its uses we can mention stitches in facial plastic surgeries, external stitches of dacriocistorrinostomy, endonasal flaps, medium ear ossicle fixation and reconstruction of ossicle chain.
Only one article has been found in the literature, referring to the use of cyanoacrylates to fix a prosthesis to ossicle chain in stapedotomy. In that article, Ribeiro et al(3). reported a fixation case of a Teflon prosthesis to incus in stapedotomy review with good result, without toxicity evidence within 4 years of follow-up, in which a patient has been submitted to a stapedotomy with Teflon prosthesis fixation to mallus after a bad result of tympanoplasty with ossicle chain reconstruction. No article referring to the use of Teflon-platinum prosthesis with a metal incus attached to it has been found.
CASE REPORTThe patient was 35 years old, married, and worked as a security guard. He had complained about a progressive and bilateral hearing loss for five years, mainly in the left. He was submitted to stapedotomy 3 years and 6 months ago, in the left year, with a good post-operatory result during the first months according to the patient himself. However, he started having important hearing loss in the same ear. He complained about left otalgy and "air bubble" tinnitus. He also confirmed a bilateral "whistle" tinnitus. He underwent a CT scan after the surgery, which did not demonstrated the prosthesis in the middle ear left or oval window.
At the physical examination, he presented otoscopy without bilateral alteration except for the cicatricial aspect of the left tympanic membrane. The test with tunning fork demonstrated indifferent Weber and bilaterally negative Rinne.
The audiometry performed during the pre-operatory phase demonstrated mixed bilateral hearing loss (Figure 1) and the immitanciometry AD curve to the left with absence of reflexes and C curve to the right with absence of reflexes.
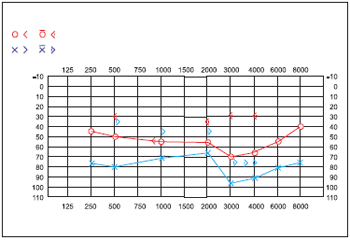
Figure 1. Pre-operatory audiometry.
After the surgery risks and possibilities have been discussed with the patient, left exploratory tympanometry has been indicated. The patient agreed on undergoing the surgery and signed the awareness term of possible complications, according to service routine. Cefazoline 2g has been prescribed with prophylactic antibioticterapy to be administered in the anesthetic. The anesthetic act proceeded without intercurrences.
The surgery proceeded under general anesthetic, and the post-operatory findings were: inspection of tympanic cleft which demonstrated adjacent fibrosis to mucosa involving the ossicular chain. Once the ossicle chain has been cleaned, a new inspection of the ossicle chain has been carried out, which showed thinning and fracture of the incus long process (distal portion), remains of crura stapes which were connected to the platinum without the remaining of the supra-stapedial structure and without the chapter. The prosthesis of the previous surgery has not been found. The platinum was rigid in the oval window. The surgery was continued. The microfenestra was carried out and a Teflon-platinum prosthesis of 7x0.45 mm has been placed in the microfenestra. It was impossible for the prosthesis nail to involve the incus body or the long process which was exiguous. The incus was then placed in the remaining of the long apophasis with HISTOACRYL
® glue and the surgery was ended after the repositioning of the tympanomeatal flap and introduction of curative.
Analgesic, antiemetic, hydration and general care have been the medication used after the surgery.
Immediately after the surgery, the patient was sleepy, but without pain. He did not complain about pain, nausea, vomit or dizziness. The surgical wound healing was clean and dry.
On the first day after the surgery, the patient presented clear vomits but no dizziness. He ate and his intestinal and vesical habits were established. He did not present nistagmus or facial paralysis. He was discharged from hospital.
On the fifteenth day after the surgery he complained he did not have significant subjective hearing improvement. He did not have otorrhea. Weber was indifferent and Rinne was bilaterally negative. Gelfoam filled the outer auditory canal.
On the first month after the surgery the stated left subjective hearing improvement, with no new symptoms. The tympanic membranes were bilaterally intact. Weber moved to the right and Rinne was positive to the left and negative to the right. A follow-up audiometry has been required.
On the third month after the surgery, He presented subjective hearing improvement to the left. He referred tinnitus like "air escape" in the left ear as well as "claps". At the otoscopy, he presented his right tympanic membrane and auditory canal without alterations and left tympanic membrane with cicatricial retraction, but intact. The audiometry showed moderate mixed loss in the right ear and mild neurosensorial loss in the left ear with deep lowering at acute frequencies (Figure 2).
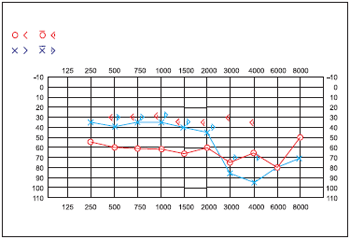
Figure 2. Post-operatory audiometry.
1 year and 4 months after the aforementioned surgery, the patient was revaluated and undertaken to a new audiometry. He maintained clinical and audiometric hearing improvement, and his new auditory examination was similar to the audiometry performed on the third month after the surgery. His physical exam also remained without changes in relation to the third-month evaluation after stapedotomy review.
DISCUSSIONStapedotomy has been considered an established surgery and by many otologic surgeons for several years, with excellent results for most of the patients who undergo to it. However, the results may not be satisfactory or even catastrophic in some situations, and may vary according to possible complications that may arise during or after the surgery. One great dilemma for the otorhinolaryngologist is the ossicle chain discontinuity or the impossibility of regularly fixating prosthesis during a stapedotomy. It is true that nowadays there are several available prosthesis which can totally or partially replace the ossicle chain. However, most of those prosthesis are not easily found here in Brazil, and are also very expensive as Ribeiro et al(3) has observed.
The fixation of the Teflon-platinum prosthesis with cyanoacrylate is more difficult when compared to the Teflon prosthesis due to the diameter of the metallic part as well as to such material's nature. We understand that the prosthesis sustaining in a conventional stapedotomy is based on the fact that the prosthesis lift involves the incus long process, thus providing stability to such prosthesis. Incase there is absence of an incus's part, such procedure becomes impossible or very difficult and the attempt to fixate the prosthesis with glue and not mechanically was an alternative which has been found before the incus long process loss. Even understanding that the adherence of cyanoacrylates to metal materials is lower than in other surfaces, a drop of glue was taken up with a otologic speculum up to the point in which the prosthesis touched the remaining of the incus long process (Figure 3). A minimum quantity of cyanoacrylate has been used and we have checked if other structures of the medium ear have not been fixated by the glue. Although the metal did not contain water, the bone tissue and ear humidity have been enough to provide cyanoacrylate polymerization.
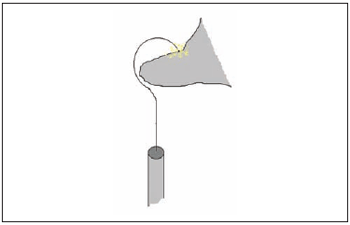
Figure 3. Schematic picture of prosthesis fixated to (remaining) incus with cyanoacrylate use.
I point out that, although the mallus was present, its size was reduced and it has not been possible to place the prosthesis in it and remain with the Teflon portion in the oval window once the prosthesis length was not enough.
Despite the little post-operatory control time, the patient evolved well, without signs of neither otologic toxicity nor side effects, even keeping the hearing gain which has been obtained after the surgery. It is important to point out that the surgery took longer than usual, even if it has been conducted by a surgeon with large experience on stapedotomies and exploratory tympanotomies. All procedure has been carried out with much care and, above all, thus avoiding the prosthesis waste, inadequate fixation and glue drying in inappropriate place and time.
There are not enough studies about ototoxicity of cyanoacrylates. However, such substances have already been used in ossicle chain reconstruction referred in the medical literature(1) and, in another article(3), with Teflon prosthesis and there is no reference of hearing loss or labyrintic symptoms which may be related to ototoxicity. For that reason, we have used such substance for prosthesis fixation.
The image recording of the performed surgery would be recommended, but equipment with technical conditions were not available for this procedure.
It is important to point out that the possibility of using cyanoacrylates in otologic surgeries has increased the number of therapeutic possibilities for surgeons in both the chain reconstruction and prosthesis fixation.
CONCLUSIONThe use of cyanoacrylates in stapedotomies with prosthesis and ossicle chain fixation is a valuable tool for otorhinolaryngologists. Other studies and case reports are necessary to better evaluate such tool. However, the case reports which have been done so far, concerning both Teflon and Teflon-platinum prosthesis, have all been successful.
BIBLIOGRAPHY1. Ronis ML, Harwick, JD, Fung R, Dellavecchia M. Review of cyanoacrylate tissue glues with emphasis ontheir otorhinolaryngological applications. Laryngoscope, 1984, 94 (2 Pt1):210-3.
2. Toriumi DM, Raslan WF, Friedman M, Tardy ME. Histotoxicity of cyanoacrylate tissue adhesives: a comparative study. Arch Otolaryngol Head Neck Surg, 1990, 116(5):546-50.
3. Ribeiro FAQ, Doria S, Almeida R. Arq Otorrinolaringol,2005 , v.9, n.1, 76-80.
4. Yarce, JC. Gastrointest Endosc. 2005 Jan;61(1):186.
5. Turler A, Wolff M, Dorlars D, Hirner A. Gastrointest Endosc. 2001 Feb;53(2):228-30.
6. Cyanoacrylate - Enpsychlopedia - May 2005. http://search.psychcentral.com/psypsych/Cyanoacrylate
7. Amarante MT, Constantinescu MA, OConnor D, Yaremchuk MJ.Cyanoacrylate fixation of the craniofacial skeleton: an experimental study. Plast Reconstr Surg. 1995 Apr;95(4):639-46.
8. Guillermo E. Chacon DDS, James P. Ellis DDS, MS, John R. Kalmar DDS, PhD and Edwin A. McGlumphy DDS, MS. Using resorbable screws for fixation of cortical onlay bone grafts: An in vivo study in rabbits. Journal of oral and maxillofacial surgery. Volume 62, Issue 11 , November 2004, Pages 1396-1402.
1. Medical Residency in Otolaryngology at HUB/UNB. Medical otorhinolaryngologist.
2 .Medical Residency in Otolaryngology at HUB/UNB. Doutorando by UNB and Harvard University.
3. Medical Residency in Otolaryngology. Medical assistant of the department of otolaryngology of the HUB/UNB.
4. Degree in Medicine. Medical Resident in Otorhinolaryngology, HUB/UNB.
5. Medical Residency in Otolaryngology at HUB/UNB. Medical Otorhinolaryngologist.
6. Expertise and PhD - University of Minesotta Post-doctoral - Massachusets, Eye and Ear In., Harvard University Medical School. Full Professor of Discipline of Otorhinolaryngology, UNB, Head of the Clinical Hospital of Otorhinolaryngology, University of Brasilia/UNB and Coordinator of the Medical Residency
Otorhinolaryngology HUB/UNB.
Institution: University Hospital of Brasilia Department of Otolaryngology and Head and Neck Surgery of.
Mailing address: SGAN 604/605 - HUB - Secretary of Clinical Cirúrgicas - Asa Norte - Brasilia/DF - CEP 70840-050 - Street Belizário Pena, 149 - Center - Barbacena/MG - Fax (32)3333-1148 - E-mail: clmvieira@yahoo.com.br
This article was submitted in PMS (Management System Publications) R @ IO in the January 11, 2006. Cod. 65. Article accepted on February 28, 2007.