INTRODUCTIONThe use and application of the three-dimensional (3D) reconstructions generated from suitable files (DICOMS) of computed tomography (CT) or magnetic resonances (MR) have been expanding recently. Such reconstructions allow physicians to observe anatomic cavities and structures of our body with an incredible amount of details and can display even the textures of different tissues (1, 2).
The applications of such reconstructions have varied from simple illustrations in exams up to the help in the diagnosis and preoperative planning in several medical specialties.
Some examples may be found in the virtual colonoscopies performed by some image centers in our country and in high resolution CTs for evaluation of the coronary arteries (3).
In our specialty there have been some attempts to carry out virtual endoscopies and laryngoscopies. However, such application has been practically abandoned due to its complexity and need for computers with high power of graphic processing (4).
However, with the evolution of proper computers and programs for reading and reconstruction of the DICOMS files, currently some authors have recovered the use of such 3D reconstructions for evaluation and preoperative planning specially related to otologic surgeries and to recess and frontal sinus (5, 6).
Such 3D reconstructions may offer potentially more usable information than those obtained with 2D views in the axial, coronal and sagittal plans. These images obtained in the three different plans: axial, coronal and sagittal are usable in the analysis of the recess and frontal sinus. However, these two-dimensional images are of more difficult comprehension for surgeons (7). BAKKER et al. Carried out a research with surgeons on what would be more difficult for learning and performance of safe nasosinusal endoscopic surgeries (8). What was considered to be more difficult for the researched surgeons to learn was: "the spatial guidance, that is, making a 3D mental representation from the 2D computed tomography". And what was taken as the second most difficult point was: "understanding the relationship between the computed tomography with endoscopic actual images" (8).
We live in a three-dimensional world and despite a large part of the endoscopes still do not allow the performance of 3D stereoscopic surgeries, the images obtained in the traditional endoscopic surgeries allow us the creation of 3D relationships in our mind. These relationships may help in the performance of specific tasks and the excellent preoperative preparation may sometimes prevent generally challenging complications (9).
We have studied the utility of the 3D reconstruction tools for the surgeries of the ear and of the recess and frontal sinus. In the literature we found since preoperative planning through other applications such as diseases staging, preoperative measurement for production of prostheses, air flow analysis and the proper teaching to resident doctors (5, 6, 8, 10).
The preoperative evaluation for the frontal sinus surgeries through 3D reconstructions from the proper CT files (DICOMS) may permit the surgeon to acquire more information than with the traditional two-dimensional images obtained with the three different plans: axial, coronal and sagittal.
Although it is possible to view all the draining pathway of the frontal sinus and of its guiding and preoperative planning through the traditional two-dimensional CT already clearly described by several authors, amongst whom WORMALD et al (9, 11), the use of 3D tools may eliminate the element of uncertainty in the correct finding of the natural draining pathway of the frontal sinus.
By using such 3D tools, it is possible to view the several holes in the region of the proper recess and send them for analysis of what is the correct hole for the frontal sinus draining.
The objective of this work consists of:
a) Demonstrating the production of such 3D reconstruction from CTs of patients submitted to nasosinusal endoscopic surgeries of the recess region and of the frontal sinus performed in a personal computer with a specific program.
b) Comparing these virtual images with actual endoscopic images during the surgery.
METHODAfter authorization of the local ethics committee, DICOM files were obtained from 10 patients taking part in the study. The inclusion criterion was of patients who were to undergo the paranasal sinuses endoscopic surgery that also included the frontal sinus. The exclusion criterion was that of patients who would not be submitted to the frontal sinus endoscopic surgery.
The folders containing files were saved in the personal computer and varied in size between 150 and 250 Mb. The CTs were requested from patients in the preoperative approach and they were carried out in different multi-slice equipment. The exams presented with cuts that varied between 0.5 and 1.3 mm of thickness.
The appropriate files (DICOMS) of the corresponding CTs were reconstructed with the computer program Intage Realia, version 2009, 0, 0, 702 (KGT Inc., Japan), by using personal computer with Microsoft Windows 7 operating system (Figure 1).
We used the following tools. The program is in English language, but we translated the tools into Portuguese for a better understanding.
1) Multiplanar reconstruction: the original DICOM files of the computed tomography are in axial plan. By using this tool, we created coronal and sagittal reconstructions with well-defined images (Figure 2). We call it three-planar or multiplanar reconstruction that is generally used in the workstations of radiologists or surgical navigators for diagnosis and surgical guiding. However, these multiplanar reconstructions did not offer 3D viewing and are generally used for the preoperative planning of patients.
2) Control of contrast, shine, shadows and segmentation: the shaded surface displays compose a tool to control shine, contrast and shadows of the images generated from the DICOM files. The alteration of these parameters enables the creation of images with different windows, which may facilitate the identification of bone tissues and soft parts. The work was carried out from the densities of the tissues and allowed us to mark and color manually or automatically (in areas of mainly aerial density) regions with osseous and aerial densities and soft parts (diseases). This segmentation tool was also important to suppress these areas of disease so that we could have a suitable view of the region studied.
3) Volume rendering: the images generated from DICOM files were transformed into 3D volume (Figure 3) that could be rotated at any plan and virtually dissected, by using a cutting tool that could also be in any plan, direction or angle, depending only on adjustments done by the computer program operator. We use this tool frequently. The volume created from the DICOM files was rotated at an angle that was compatible with the entering of the patient to the surgery. As from this plan, dissections were made by the volume both in the upper and the lower direction with the densities of the osseous and aerial areas and soft parts marked with different colors. This allowed us a 3D viewing of the recess region of the frontal sinus that enables a detailed study of the possible draining channels of the frontal sinus.
4) Fly through: this tool allowed us navigation within the volume created, that simulates an endoscopical image or a virtual endoscopy (Figure 4). From commands on the computer program, selecting the option VE (virtual endoscopy), we obtain an endoscopic viewing of the ostia of the frontal recess. In patients with less disease in the frontal sinus (mucosa edema, etc.) we could more easily perform this task in less time because we do not need to segment and/or suppress diseased areas.
With virtual endoscopy it was important to keep a guideline that should be the same as that used in endoscopic surgeries or actual endoscopies.
The available tools in this program also allowed the moving of the virtual camera and changing of its angles so that we could reach limited spaces, which would not be possible with actual endoscopy.
The starting point for fly through virtual endoscopy was the region of the middle meatus, between the uncinated process, ethmoidal bulla and middle infundibulum. After this initial layout, the view field was moved upwards the frontal sinus recess. As we advanced, several apparent holes appeared. We mapped this ostia configuration and captured the screen to compare the endoscopic view obtained from actual surgeries.
After this 3D reconstruction study, the surgery was digitally performed and stored. The actual endoscopic images of the recess and frontal sinus region were compared to images generated from the personal computer to evaluate the likeness.
RESULTSThe 3D reconstruction and the virtual endoscopy were performed in all 10 patients who were later submitted to the recess and frontal sinus endoscopic surgery.
The images generated in the computer had a large visual resemblance with the images found in the actual surgeries (Figures 5, 6 and 7).
Such reconstructions were made without major technical difficulties from a personal computer, by using the appropriate program for reading and edition of DICOM files.
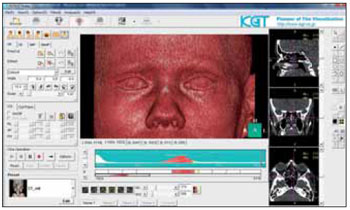
Figure 1. Image of the control screen of the software used.
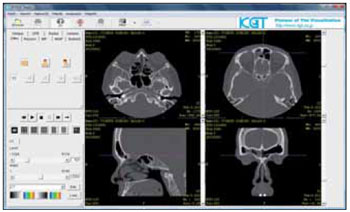
Figure 2. Image captured from the computer screen with the program showing coronal and sagittal reconstruction, that is, the images in the three plans (triplanar), in 2D though.
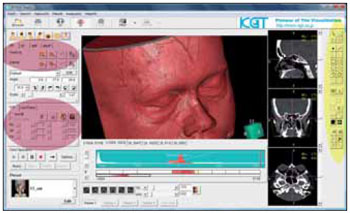
Figure 3. Image of the computer with a program showing 3D volume rendering. In the purple ellipses we may view the commands for virtual "dissection", free cuts and controls for rotation and guiding of this 3D volume. Refer to the yellow ellipsis with commands for selection (that may be manual or automatic) of areas both in 2D and 3D volume reconstructions, for further segmentation and/or suppression of some densities.
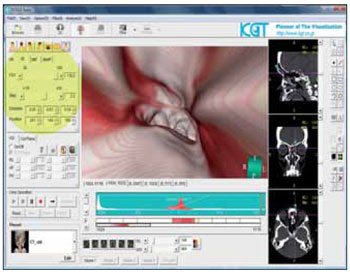
Figure 4. Image showing example of virtual endoscopy, in the VE command. Refer to the possibility of fly through and different image angles (that may range from 30 to 120 degrees).
The standard of the holes in the frontal recess area is quite variable and the exact location of the natural drainage of this sinus is not easily determined by the traditional two-directional anatomic cuts found in a CT (axial, coronal and sagittal) (7, 9, 11, 12).
In case of an extensive disease this becomes even more difficult. With 3D reconstruction from the proper CT files of the patients, we could make a virtual map of the frontal sinus recess region, by evaluating the ostia configuration and the correct pathway for natural drainage of the frontal sinus. However, in these cases in which we found very extensive diseases in the sinus and frontal recess region, the identification of the correct drainage pathway of the frontal sinus was difficult, even with 3D reconstructions, since for the execution of the virtual endoscopies some presence of air in the cavities for a better guidance and navigation is required. In these cases, we were guided directly by the osseous part or used special tools for rendering and suppression of the diseased areas.
For the correct location of the recess and frontal sinus region, we began by trying to identify the Agger Nasi that was present in all cases studied and reconstructed. This is typically the first ethmoidal cell seen in the coronal plan at the antero-posterior direction and is typically confluent with the uncinated process (12).
The second step was to select the software endoscopic viewpoint with the correct guiding, that is, the same guiding used for traditional surgeries, for the area between the uncinated process, the ethmoidal bulla and the middle infundibulum. From this point, we moved the vision field upwards the frontal sinus and mapped the ostia configuration so that we could learn in which hole the natural draining of the frontal sinus was.
We had previously attempted to locate the frontal sinus natural draining pathway through common cuts (2D) of computed tomographies. However, even trying to connect the images in axial, coronal and sagittal plans, it was too difficult to find the exact way for natural draining of the frontal sinus.
It is worth remarking that these 3D reconstructions from the CT-proper DICOMS files of the patients may also be made in other personal computers with another operating system, such as MacintoshTM, of AppleTM, in a suitable program called OsiriXTM, and the possible performance of virtual otoscopy and preoperative planning for larynx and ear surgeries.
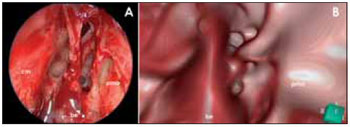
Figure 5. Comparison of real with virtual endoscopy image. A: real endoscopy (30 degrees instrument) of the left frontal sinus recess region. Cm: middle infundibulum; be: Ethmoidal bulla; pmo: medial wall of the orbit. B: virtual endoscopy of the same region. Refer to resemblance of the images.
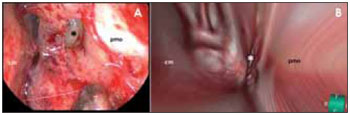
Figure 6. Comparison of real with virtual endoscopy image. A: real endoscopy (30 degrees instrument) of the left frontal sinus recess region. Cm: middle infundibulum; pmo: medial wall of the orbit. B: virtual endoscopy of the same region. Refer to resemblance of the images.
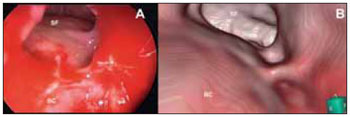
Figure 7. Comparison of real with virtual endoscopy image. A: real endoscopy (45-degree instrument) of the frontal sinus (SF) region of the patient after opening. BC: cranial base in the frontal-ethmoidal angle region. B: virtual endoscopy of the same region. Refer to resemblance of the images.
With relatively simple tools and personal computer, we demonstrated the possibility to generate 3D reconstructions and virtual endoscopies from DICOM files of patients' CP. In these patients submitted to surgery with the study of the previous 3D reconstruction, the frontal sinus was accessed in all cases. However, it is notorious that we did not performed comparative studies with a group of patients in which no 3D reconstruction was made.
The preoperative knowledge of the frontal sinus natural draining path location may generate significant benefits during the performance of surgeries such as shorter surgical time and stronger safety for the patients. Nevertheless, it is worth taking into account that more studies must be developed for the evaluation of the real roles of such 3D reconstructions and virtual endoscopies.
BIBLIOGRAPHICAL REFERENCES1. Anand SM, Frenkiel S, Le BQ, et al. Virtual endoscopy: our next major investigative modality? J Otolaryngol Head Neck Surg. 2009, 38(6):642-5.
2. Wood BJ, Razavi P. Virtual endoscopy: a promising new technology. Am Fam Physician. 2002, 66(1):107-12.
3. McSweeney SE, ODonoghue PM, Jhaveri K. Current and emerging techniques in gastrointestinal imaging. J Postgrad Med. 2010, 56(2):109-16.
4. Gilani S, Norbash AM, Ringl H, et al. Virtual endoscopy of the paranasal sinuses using perspective volume rendered helical sinus computed tomography. Laryngoscope. 1997, 107(1):25-9.
5. Schulze F, Bühler K, Neubauer A, et al. Intra-operative virtual endoscopy for image guided endonasal transsphenoidal pituitary surgery. Int J Comput Assist Radiol Surg. 2010, 5(2):143-54.
6. Lee WT, Kuhn FA, Citardi MJ. 3D computed tomographic analysis of frontal recess anatomy in patients without frontal sinusitis. Otolaryngol Head Neck Surg. 2004, 131(3): 164-73.
7. Pletcher SD, Hoxworth JM, Goldberg AN, et al. Computed tomography imaging of the paranasal sinuses: direct versus reformatted coronal images. Otolaryngol Head Neck Surg. 2008, 138(6):710-4.
8. Bakker NH, Fokkens WJ, Grimbergen CA. Investigation of training needs for functional endoscopic sinus surgery (FESS). Rhinology. 2005, 43(2):104-8.
9. Wormald PJ. Three-dimensional building block approach to understanding the anatomy of the frontal recess and frontal sinus. Operative techniques in Otolaryngology. 2006, 17: 2-5.
10. Krüeger A, Kubisch C, Straub G, et al. Sinus endoscopy-application of advanced GPU volume rendering for virtual endoscopy. IEEE Trans Vis Comput Graph. 2008, 14(6):1491-8.
11. Wormald PJ. Surgery of the frontal recess and frontal sinus. Rhinology. 2005, 43(2):82-5.
12. Park SS, Yoon BN, Cho KS, et al. Pneumatization Pattern of the Frontal Recess: Relationship of the Anterior-to-Posterior Length of Frontal Isthmus and/or Frontal Recess with the Volume of Agger Nasi Cell. Clin Exp Otorhinolaryngol. 2010, 3(2):76-83.
1 Master's Degree in Medicine. Resident of the 3rd Year of Otorhinolaryngology of the General Hospital of Fortaleza - HGF.
2 Specialist in Otorhinolaryngology from ABORL-CCF Director of the Sinus Centro Otorhinolaryngologist of the General Hospital of Fortaleza - HGF.
3 Bachelor Degree in Medicine. Resident of the 2nd Year of Otorhinolaryngology of the General Hospital of Fortaleza - HGF.
4 Bachelor Degree in Medicine. Resident of the 1st Year of Otorhinolaryngology of the General Hospital of Fortaleza - HGF.
Institution: Hospital Geral de Fortaleza - HGF & Sinus Centro. Fortaleza / CE - Brazil. Mail address: João Flávio Nogueira - Avenida Pontes Vieira, 2531 - Bairro: São João do Tauape - Fortaleza / CE - Brazil - Telefone: (+55 85) 8152-2322 - http://www.sinuscentro.com.br - E-mail: joaoflavioce@hotmail.com
Article received on September 1, 2010. Approved on October 7, 2010.