 |
453 |
|
| Year: 2007 Vol. 11 Num. 3 - Jul/Set - (20º)
|
|
 |
|
|
|
| Author(s): |
| Guilherme Luís da Silva Franche1, Fernanda Batesini Da Cas2, Eduardo Homrich Granzotto3, Andresa Thier de Borba4, Lucas Hemb4, Cátia de Souza Saleh5
|
|
|
| Key words: |
| Meningioma. Surgery. Paranasal sinuses. |
|
|
 |
| Abstract: |
Introduction: Meningiomas account for nearly 20% of all intracranial neoplasms and are the second most common tumors of the central nervous system (following gliomas). However, primary meningiomas of the paranasal sinuses are extremely rare. The clinical and radiological features of these tumors are nonspecific, and consequently an accurate diagnosis requires histologic evaluation. Objective: To report a case of nasal meningioma. Case Report: A 48 years old female, black, presented to our service in March of 2000, complaining of nasal obstruction
associate with festering secretion with blood lines. Former rinoscopic examination revealed soft mass in left nasal cavity between the septum and the turbinates. Computed tomography (CT) revealed the presence of a material with soft parts density in the nasal cavity (middle meatus) and the ethmoid maze. The biopsy of the lesion revealed fusiform cells neoplasm in the chorion of breathing mucosa, therefore meningioma was suspected. The patient underwent a nasal endoscopic surgery and had a good transoperative and postoperative course. After 5 years of follow-up, the patient is asymptomatic, with normal nasal endoscopic examination and no sign of recurrence. Final Comment: Meningiomas involving the nasal cavity and paranasal sinuses are rare. The mortality is low, and its lethality is due to the complications of the surgery and injury of vital structures. Complete surgical extirpation of the sinonasal tract meningiomas has an overall good prognosis. Hence, endoscopic nasal approach is an excellent surgical option in these cases, due to its low morbidity and satisfactory lesion resection.
|
|
 |
INTRODUCTION
Meningioma is an ordinary intracranial neoplasm, with a histomorphological development standard and, in general, easily recognized. Therefore, primary extracranial meningiomas of nasal cavity, paranasal sinus and of nasopharinx are rare. Literature and its review is usually limited regarding isolated case reports (1).
Meningiomas accounts for nearly 20% of all intracranial neoplasms, and they are the second most common tumors of the central nervous system (following gliomas). However, primary meningiomas of the paranasal sinuses are extremely rare. Only 30 cases have been previously reported in English (2).
Meningiomas arise from meningothelial arachnoid cells which derive from neuroectodermal tumors. Therefore, they are usually classified as mesoderm tumors (2).
The current study reports a case of nasal meningioma of a patient who searched Serviço de Otorrinolaringologia do Complexo Hospitalar Santa Casa.
CASE REPORT
A 48-year-old, black skin female, searched Serviço de Otorrinolaringologia do Complexo Hospitalar Santa Casa in March,2000 complaining of nasal obstruction associated with festering secretion with blood lines. Former rhinoscopic examination revealed lesion on left nasal fossa (LNF) between septum and tubinates. Computed tomography (CT) revealed the presence of a material with soft part density in the nasal cavity (middle meatus) and the ethmoid labyritnh. (Pictures 1 and 2). The biopsy of the lesion revealed fusiform cell neoplasm in the chorion of breathing mucosa, therefore matching meningioma.
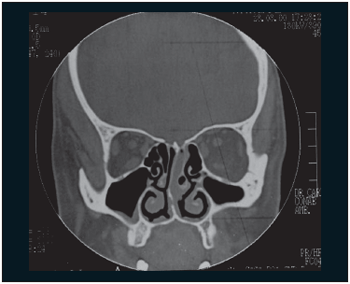 Picture 1. Tomography in coronal cut displaying a veiling of nasal fossa ceiling between middle concha and nasal septum, to the left. 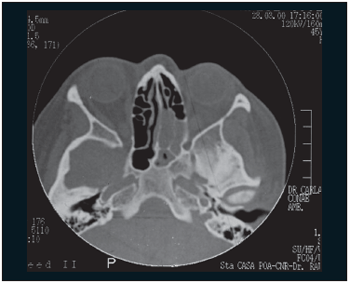 Picture 2. Tomography in axial cut displaying a veiling of posterior ethmoid cells, of the sphenoid and nasal fossa, to the left.
Patient underwent nasal endoscopic surgery in September, 2000. She presented good postoperative development with no complications or intercurrences. In March 2001, she had no complaints and nasal endoscopy revealed no lesions or recurrences signs with ostium of free sphenoid sinus.
In 2005, five years after surgery, patient remained assymtomatic, with normal nasal endoscopic examination and no sign of recurrence.
DISCUSSION
Meningiomais is well-known as a tumor of the central nervous system, but lately it has been occurring as a primary extracranial tumor of the paranasal sinuses (2).
Meninigomas affecting paranasal and nasal cavity is rare. They occur as a result of an extension of a primary intracranial mass, affecting only around 3% of the cases, so it not a common event. Such tumors can also be reported with no evidence of intracranial tumor. Their origin is uncertain, including the origin of arachnoid cells around nerves or heterotopic cells when displaced in the moment of the structure closing of the embryo´s midline. The origin of Schwann cells or mesenchyme pluripotential ones is also suggested (3).
Regarding the head and neck area, primary extracranial meningiomas were reported on the bones of the skull, orbit, temporal bone, inner ear, nasal cavity and paranasal sinuses. They are classified as:
- Extracranial extension of meningioma with intracranial origin;
- Extracranial extension of meningioma which arouse on neural foramen;
- Primary and ectopic extracranial meningioma with no relation with foramen of cranial nerve or with endocranium;
- Extracranial metastasis of intracranial meningioma for parapharyngeal lymph node (2).
A variety of signs and symptoms are reported regarding clinical terms, including nasal obstruction and secretion, nasal polyps, maxillary pain, periorbital oedema, exophtalmia, proptosis, ptosis, sight reduction, hearing loss and headache (3).
Regarding histology, meningotheliomas is reported, i.e, lobule cells with irregular outline and nucleolus increased by visible roseate chromatin, besides more common transitional cells and psamomas bodies in its interior (4).
Transitional meningiomas are a very common type of such tumor (75% of cases), followed by synsytial and fibrous tumors (10% each), angioblásticos (5%) e sarcomatosos (<1%) (2).
There is a range of benign and malignent neoplasm in the differential diagnosis of sinonasal tract meningiomas, including epithelial tumors (carcinomas), neurogenic tumors (melanoma and olfactory neuroblastoma), vascular tumors (angiofibroma and paraganglioma) and tumors of mesenquimal tissues (aggressive psammomatous ossified fibroma) (1).
Prognosis of primary meningiomas of sinonasal tract is excellent with patient survival rate raging between 82.1% and 78.6% in 5 and 10 years, respectively. Metastasis from this tumor was not found in the literature. Mortality rate is not expressively reported by surgery complications and lesion of vital structures (1).
Diagnosis is performed with the exam of pathological material. Such neoplasm, involving nasal cavity or paranasal sinus is common and its development is slow. When surgically removed, primary meningiomas prognosis of nasal cavity is favorable with low rate of reported recurrences. Therefore, prognosis of patients with intracranial involvement is less favorable (3).
Wide margin surgical removal is the chosen therapy (5). Side therapy, such as radiotherapy was not efficient not even for disease recurrence (1).
SWAIN et al. have found three cases of paranasal sinus meningiomas, including frontal, ethmoid and sphenoid sinus when revising a retrospective study in the past 25 years.
SCIARRETTA et al. have revised 33 cases of benign tumors of paranasal sinus, and meningioma was one of them, in which they evaluate the efficacy of endoscopic surgery therapy. Following them, authors reported 6% of recurrence and concluded that endoscopic surgery, in some cases, can be considered an effective therapy for resection of benign tumors of the sinonasal tract (7). The reported case in the current study was also submitted to an endoscopy surgery. It was followed up for 36 months and did not present recurrence.
FINAL COMMENTS
Meningiomas of sinonasal tract are uncommon lesions. The clinical and radiologic criteria of such tumors are unspecified, and so, acute diagnosis requires histological evaluation. Meningiomas of sinonasal tract are histologically and immunophenotypically undistinguishable from intracranial ones. Pathological features and immune-histochemical criteria enable distinguishion among those neoplasms and other tumors of sinonasal tract. Comprehensive surgical resection in meningiomas of sinosal tract is usually well prognosticated (1).
REFERENCES
1. Thompson LDR, LCDR, MC, USNR; Gyure A. Extracranial Sinonasal Tract Meningiomas: A Clinicopathologic Study of 30 Cases With a Review of the Literature Am J Surg Pathol. 2000, May;24(5):640-50.
2. Daneshi A, Asghari A, Bahramy E. Primary meningeoma of the ethmoid sinus: a case report. ENT- Ear, Nose & Throat Journal, 2003 April, 82(4):310-311.
3. Mccullough JB, Evans AT, Vaughan-Jones R, Hussein KA. Fine needle aspiration (FNA) of a nasal meningioma: a case report. Cytopathology, 1996, 7, 56-60.
4. Daneshi A., Asghari A, Bahramy E. Primary meningioma of the ethmoid sinus: a case report. Ear Nose Throat J. 2003, Apr;82(4):310-1.
5. Couldwell WT, Weiss MH, Rabb C, Liu JK, Apfelbaum RI, Fukushima T. Variations on the standard transsphenoidal approach to the sellar region, with emphasis on the extended approaches and parasellar approaches: surgical experience in 105 cases. Neurosurgery. 2004 Sep;55(3):539-47; discussion 547-50.
6. Swain REJ, Kingdom TT, DelGaudio JM, Muller S, Grist WJ. Meningiomas of the paranasal sinuses. Am J Rhinol. 2001, Jan-Feb;15(1):27-30.
7. Sciarretta V, Pasquini E, FranK G, Modugno GC, Cantaroni C, Mazzatenta D, et al. Endoscopic treatment of benign tumors of the nose and paranasal sinuses: a report of 33 cases. Am J Rhinol. 2006J, an-Feb;20(1):64-71.
1 Masters in Medicine from the Federal University of Rio Grande do Sul (Cooordenador of Ambulatory Rinologia of the Office of the DSB Hospital Complex Santa
Casa de Porto Alegre).
2 Formed by the Medical University of Passo Fundo-RS (Medical).
3 Medical Resident of the Office of Otorhinolaryngology, Santa Casa Hospital Complex - Porto Alegre. (Medical Resident 3 of the Year of Otorhinolaryngology).
4 Medical Resident of the Office of Otorhinolaryngology, Santa Casa Hospital Complex - Porto Alegre. (Medical Resident 2 of the Year in Otolaryngology).
5 Academic Faculty of Medicine of the Federal Foundation of Medical Sciences of Porto Alegre (of Academic Medicine).
Institution: Department of Otorhinolaryngology, Santa Casa Hospital Complex - Porto Alegre / RS.
Mailing address: Luis Guilherme da Silva Franche - Street Mostardeiro 333/508 - Neighborhood Moinhos de Vento - Porto Alegre / RS - CEP 90430-001 -- Fax: (51) 3343-1415 - E-mail: gfranche@redemeta.com.br
This article was submitted in Management System Publications in the R@IO 24/10/2006 20:38:54 and approved on 19/12/2006 21:49:54.
|
|
 |
|
|
